Implementation of a Delirium Bundle for Pediatric Intensive Care Patients
- PMID: 35198518
- PMCID: PMC8859429
- DOI: 10.3389/fped.2022.826259
Implementation of a Delirium Bundle for Pediatric Intensive Care Patients
Abstract
Background and objective: Delirium represents the most common form of acute cerebral dysfunction in critical illness. The prevention, recognition, and treatment of delirium must become the focus of modern pediatric intensive care, as delirium can lead to increased morbidity and mortality. The aim of this study is to evaluate the impact of a delirium bundle consisting of mainly non-pharmacological measures.
Material and methods: This is a pre-/post-implementation study in an interdisciplinary pediatric intensive care unit of a tertiary care university hospital. In the pre-implementation period, pediatric intensive care delirium was monitored using the Sophia Observation withdrawal Symptoms and Pediatric Delirium scale. After introduction of a delirium bundle consisting of non-pharmacological prevention and treatment measures a period of 4 months was interposed to train the PICU staff and ensure that the delirium bundle was implemented consistently before evaluating the effects in the post-implementation period. Data collection included prevalence of delirium and withdrawal, length of PICU stay, duration of mechanical ventilation, and cumulative dose of sedatives and analgesics.
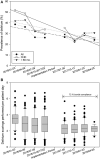
Results: A total of 792 critically ill children aged 0-18 years were included in this study. An overall delirium prevalence of 30% was recorded in the pre-implementation group and 26% in the post-implementation group (p = 0.13). A significant reduction in the prevalence of pediatric delirium from was achieved in the subgroup of patients under 5 years of age (27.9 vs. 35.8%, p = 0.04) and in patients after surgery for congenital heart disease (28.2 vs. 39.5%, p = 0.04). Young age, length of PICU stay, and iatrogenic withdrawal syndrome were found to be risk factors for developing delirium.
Conclusions: Based on a validated delirium monitoring, our study gives new information regarding the prevalence of pediatric delirium and the characteristics of intensive care patients at risk for this significant complication. Especially young patients and patients after surgery for congenital heart disease seem to benefit from the implementation of non-pharmacological delirium bundles. Based on our findings, it is important to promote change in pediatric intensive care-toward a comprehensive approach to prevent delirium in critically ill children as best as possible.
Keywords: PICU; PICU delirium bundle; analgesia; critical care; delirium; post-intensive care syndrome; sedation; withdrawal.
Copyright © 2022 Michel, Schepan, Hofbeck, Engel, Simma and Neunhoeffer.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


References
-
- American Psychiatric Association . Diagnostic and Statistical Manual of Mental Disorders. Washington, DC: American Psychiatric Association; (1980).
LinkOut - more resources
Full Text Sources

