Prognostic indicators of arthroscopic discopexy for management of temporomandibular joint closed lock
- PMID: 35210483
- PMCID: PMC8873273
- DOI: 10.1038/s41598-022-07014-9
Prognostic indicators of arthroscopic discopexy for management of temporomandibular joint closed lock
Abstract
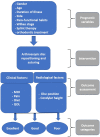
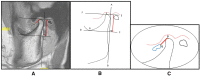
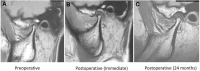
In order to optimize patient selection for temporomandibular joint (TMJ) arthroscopic discopexy to achieve favorable outcomes, prognostic indicators impacting the results are important to analyze. This longitudinal retrospective study aimed to analyze various prognostic factors impacting surgical outcomes following arthroscopic discopexy for management of TMJ closed lock using success criteria based on pain, maximal interincisal opening, diet, and quality of life. Furthermore, a quantitative MRI assessment was performed pre- and post-operatively. Multivariate analysis was used to evaluate various prognostic variables including gender, age, side, duration of illness, Wilkes staging, parafunctional habits, splint therapy and orthodontic treatment. A total of 147 patients (201 joints) were included. The outcome was categorized as excellent (n = 154/76.61%), good (n = 34/16.91%), or poor (n = 13/6.46%) with a success rate of 93.54%. Patients aged > 30 years old (p = 0.048), longer duration of illness (12-24 months: p = 0.034) and (> 24 months: p = 0.022), and patients with Wilkes stage IV (p = 0.002) were all significantly more likely to be in the poor outcome group. Finally, orthodontic treatment showed a significant association with excellent outcomes (p = 0.015). Age, duration of illness, Wilkes staging, and orthodontic treatment are considered significant prognostic factors that can predict the outcomes following the arthroscopic discopexy for management of TMJ closed lock.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
Arthroscopic discopexy is effective in managing temporomandibular joint internal derangement in patients with Wilkes stage II and III.J Oral Maxillofac Surg. 2015 Mar;73(3):391-401. doi: 10.1016/j.joms.2014.09.004. Epub 2014 Sep 21. J Oral Maxillofac Surg. 2015. PMID: 25530277 Clinical Trial.
-
Intraoperative complications in temporomandibular joint arthroscopy: A retrospective observational analysis of 899 arthroscopies.J Craniomaxillofac Surg. 2022 Aug;50(8):651-656. doi: 10.1016/j.jcms.2022.06.011. Epub 2022 Jul 8. J Craniomaxillofac Surg. 2022. PMID: 35842375
-
Clinical and demographic factors associated with the effectiveness of temporomandibular joint arthroscopy.Oral Maxillofac Surg. 2024 Mar;28(1):405-411. doi: 10.1007/s10006-023-01158-2. Epub 2023 May 24. Oral Maxillofac Surg. 2024. PMID: 37222837
-
Comparison of the TMJ arthroscopy discopexy techniques: A systematic review and meta-analysis.J Craniomaxillofac Surg. 2024 May;52(5):558-564. doi: 10.1016/j.jcms.2024.04.004. Epub 2024 Apr 16. J Craniomaxillofac Surg. 2024. PMID: 38631972
-
Arthroscopic Disc Repositioning Techniques of the Temporomandibular Joint Part 2: Resorbable Pins.Atlas Oral Maxillofac Surg Clin North Am. 2022 Sep;30(2):185-191. doi: 10.1016/j.cxom.2022.06.011. Atlas Oral Maxillofac Surg Clin North Am. 2022. PMID: 36116877 Review.
Cited by
-
Recent Advances in Temporomandibular Joint Surgery.Medicina (Kaunas). 2023 Aug 2;59(8):1409. doi: 10.3390/medicina59081409. Medicina (Kaunas). 2023. PMID: 37629699 Free PMC article. Review.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

