Evaluating the Impact of Orthostatic Syncope and Presyncope on Quality of Life: A Systematic Review and Meta-Analysis
- PMID: 35224062
- PMCID: PMC8866568
- DOI: 10.3389/fcvm.2022.834879
Evaluating the Impact of Orthostatic Syncope and Presyncope on Quality of Life: A Systematic Review and Meta-Analysis
Abstract
Purpose: Syncope (transient loss of consciousness and postural tone) and presyncope are common manifestations of autonomic dysfunction that are usually triggered by orthostasis. The global impact of syncope on quality of life (QoL) is unclear. In this systematic review, we report evidence on the impact of syncope and presyncope on QoL and QoL domains, identify key factors influencing QoL in patients with syncopal disorders, and combine available data to compare QoL between syncopal disorders and to population normative data.
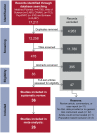
Methods: A comprehensive literature search of academic databases (MEDLINE (PubMed), Web of Science, CINAHL, PsycINFO, and Embase) was conducted (February 2021) to identify peer-reviewed publications that evaluated the impact of vasovagal syncope (VVS), postural orthostatic tachycardia syndrome (POTS), or orthostatic hypotension (OH) on QoL. Two team members independently screened records for inclusion and extracted data relevant to the study objectives.
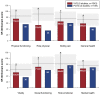
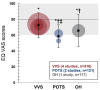
Results: From 12,258 unique records identified by the search, 36 studies met the inclusion criteria (VVS: n = 20; POTS: n = 13; VVS and POTS: n = 1; OH: n = 2); 12 distinct QoL instruments were used. Comparisons of QoL scores between patients with syncope/presyncope and a control group were performed in 16 studies; significant QoL impairments in patients with syncope/presyncope were observed in all studies. Increased syncopal event frequency, increased autonomic symptom severity, and the presence of mental health disorders and/or comorbidities were associated with lower QoL scores.
Conclusion: This review synthesizes the negative impact of syncope/presyncope on QoL and identifies research priorities to reduce the burden of these debilitating disorders and improve patient QoL.
Keywords: carotid sinus hypersensitivity; orthostatic hypotension; postural orthostatic tachycardia syndrome (POTS); quality of life; vasovagal syncope.
Copyright © 2022 Hockin, Heeney, Whitehurst and Claydon.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

