Optimal effectiveness of heart failure management - an umbrella review of meta-analyses examining the effectiveness of interventions to reduce (re)hospitalizations in heart failure
- PMID: 35239106
- PMCID: PMC8892116
- DOI: 10.1007/s10741-021-10212-8
Optimal effectiveness of heart failure management - an umbrella review of meta-analyses examining the effectiveness of interventions to reduce (re)hospitalizations in heart failure
Abstract
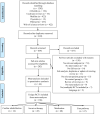
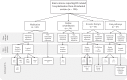
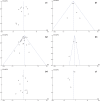
Heart failure (HF) is a major health concern, which accounts for 1-2% of all hospital admissions. Nevertheless, there remains a knowledge gap concerning which interventions contribute to effective prevention of HF (re)hospitalization. Therefore, this umbrella review aims to systematically review meta-analyses that examined the effectiveness of interventions in reducing HF-related (re)hospitalization in HFrEF patients. An electronic literature search was performed in PubMed, Web of Science, PsycInfo, Cochrane Reviews, CINAHL, and Medline to identify eligible studies published in the English language in the past 10 years. Primarily, to synthesize the meta-analyzed data, a best-evidence synthesis was used in which meta-analyses were classified based on level of validity. Secondarily, all unique RCTS were extracted from the meta-analyses and examined. A total of 44 meta-analyses were included which encompassed 186 unique RCTs. Strong or moderate evidence suggested that catheter ablation, cardiac resynchronization therapy, cardiac rehabilitation, telemonitoring, and RAAS inhibitors could reduce (re)hospitalization. Additionally, limited evidence suggested that multidisciplinary clinic or self-management promotion programs, beta-blockers, statins, and mitral valve therapy could reduce HF hospitalization. No, or conflicting evidence was found for the effects of cell therapy or anticoagulation. This umbrella review highlights different levels of evidence regarding the effectiveness of several interventions in reducing HF-related (re)hospitalization in HFrEF patients. It could guide future guideline development in optimizing care pathways for heart failure patients.
Keywords: Care pathways; Heart failure related hospitalizations; Interventions; Invasive therapy; Medication; Rehabilitations.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures








References
-
- Magnussen C, Niiranen TJ, Ojeda FM, Gianfagna F, Blankenberg S, Vartiainen E, Sans S, Pasterkamp G, Hughes M, Costanzo S, Donati MB, Jousilahti P, Linneberg A, Palosaari T, de Gaetano G, Bobak M, den Ruijter HM, Jørgensen T, Söderberg S, Kuulasmaa K, Zeller T, Iacoviello L, Salomaa V, Schnabel RB. Sex-specific epidemiology of heart failure risk and mortality in Europe: results from the BiomarCaRE consortium. JACC Hear Fail. 2019;7:204–213. doi: 10.1016/j.jchf.2018.08.008. - DOI - PubMed
-
- Mamas MA, Sperrin M, Watson MC, Coutts A, Wilde K, Burton C, Kadam UT, Kwok CS, Clark AB, Murchie P. Do patients have worse outcomes in heart failure than in cancer? a primary care-based cohort study with 10-year follow-up in Scotland. Eur J Heart Fail Wiley Online Library. 2017;19:1095–1104. doi: 10.1002/ejhf.822. - DOI - PubMed
-
- Data from the American Heart Association (2000) Heart and stroke statistical update. Am Hear Assoc Dallas. TX
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

