Effect of uncultured adipose-derived stromal vascular fraction on preventing urethral stricture formation in rats
- PMID: 35246575
- PMCID: PMC8897427
- DOI: 10.1038/s41598-022-07472-1
Effect of uncultured adipose-derived stromal vascular fraction on preventing urethral stricture formation in rats
Abstract
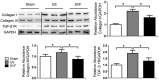
Urethral stricture (US) remains a challenging disease without effective treatment options due to the high recurrence rate. This study aims to evaluate the preventive effect of uncultured adipose derived stromal vascular fraction (SVF) on urethral fibrosis in a rat model of US. Results demonstrated that US rats displayed hyperechogenic urethral wall with a narrowed lumen compared with sham rats, while SVF rats exhibited less extensive urethral changes. By histology, US rats showed obvious submucosal fibrosis in the urethral specimens, while SVF rats exhibited mild submucosal fibrosis with less extensive tissue changes. Furthermore, US rats showed increased gene and protein expression of collagen I (2.0 ± 0.2, 2.2 ± 0.2, all were normalized against GAPDH, including the following), collagen III (2.5 ± 0.3, 1.2 ± 0.1), and TGFβ1R (2.8 ± 0.3, 1.9 ± 0.2), while SVF cells administration contributed to decreased gene and protein expression of collagen I (1.6 ± 0.2, 1.6 ± 0.2), collagen III (1.8 ± 0.4, 0.9 ± 0.1), and TGFβ1R (1.8 ± 0.3, 1.3 ± 0.2), in parallel with the improvement of vascularization and increased expression of VEGF (1.7 ± 0.1) and bFGF (3.1 ± 0.3). Additionally, SVF served anti-inflammatory effect through regulation of inflammatory cytokines and cells, accompanied with conversion of the macrophage phenotype. Our findings suggested that uncultured SVF presented an inhibitory effect on stricture formation at an early stage of urethral fibrosis.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



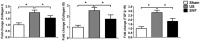



Similar articles
-
Cell sheet formation enhances the therapeutic effects of adipose-derived stromal vascular fraction on urethral stricture.Mater Today Bio. 2024 Feb 29;25:101012. doi: 10.1016/j.mtbio.2024.101012. eCollection 2024 Apr. Mater Today Bio. 2024. PMID: 38464495 Free PMC article.
-
Adipose-derived Stem Cells Counteract Urethral Stricture Formation in Rats.Eur Urol. 2016 Dec;70(6):1032-1041. doi: 10.1016/j.eururo.2016.04.022. Epub 2016 May 3. Eur Urol. 2016. PMID: 27156445
-
Human uncultured adipose-derived stromal vascular fraction shows therapeutic potential against osteoarthritis in immunodeficient rats via direct effects of transplanted M2 macrophages.Stem Cell Res Ther. 2024 Sep 27;15(1):325. doi: 10.1186/s13287-024-03946-3. Stem Cell Res Ther. 2024. PMID: 39334434 Free PMC article.
-
Adipose tissue-derived stromal vascular fraction in regenerative medicine: a brief review on biology and translation.Stem Cell Res Ther. 2017 Jun 15;8(1):145. doi: 10.1186/s13287-017-0598-y. Stem Cell Res Ther. 2017. PMID: 28619097 Free PMC article. Review.
-
Adipose-Derived Stromal Vascular Fraction Cells: Update on Clinical Utility and Efficacy.Crit Rev Eukaryot Gene Expr. 2015;25(2):145-52. doi: 10.1615/critreveukaryotgeneexpr.2015013057. Crit Rev Eukaryot Gene Expr. 2015. PMID: 26080608 Review.
Cited by
-
Overexpressed miR-486 in bone marrow mesenchymal stem cells represses urethral fibrosis and targets Col13a1 in urethral stricture rats.J Cell Commun Signal. 2024 Apr 22;18(2):e12028. doi: 10.1002/ccs3.12028. eCollection 2024 Jun. J Cell Commun Signal. 2024. PMID: 38946723 Free PMC article.
-
The Effect of Tissue Stromal Vascular Fraction as Compared to Cellular Stromal Vascular Fraction to Treat Anal Sphincter Incontinence.Bioengineering (Basel). 2022 Dec 26;10(1):32. doi: 10.3390/bioengineering10010032. Bioengineering (Basel). 2022. PMID: 36671604 Free PMC article.
-
Cell sheet formation enhances the therapeutic effects of adipose-derived stromal vascular fraction on urethral stricture.Mater Today Bio. 2024 Feb 29;25:101012. doi: 10.1016/j.mtbio.2024.101012. eCollection 2024 Apr. Mater Today Bio. 2024. PMID: 38464495 Free PMC article.
-
The Regenerative Microenvironment of the Tissue Engineering for Urethral Strictures.Stem Cell Rev Rep. 2024 Apr;20(3):672-687. doi: 10.1007/s12015-024-10686-7. Epub 2024 Feb 2. Stem Cell Rev Rep. 2024. PMID: 38305981 Review.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials

