Long-Term Blood Pressure Variability and Major Adverse Cardiovascular and Cerebrovascular Events After Intracerebral Hemorrhage
- PMID: 35253479
- PMCID: PMC9075304
- DOI: 10.1161/JAHA.121.024158
Long-Term Blood Pressure Variability and Major Adverse Cardiovascular and Cerebrovascular Events After Intracerebral Hemorrhage
Abstract
Background Survivors of intracranial hemorrhage (ICH) are at increased risk for major adverse cardiovascular and cerebrovascular events (MACCE), in the form of recurrent stroke and myocardial Infarction. We investigated whether long-term blood pressure (BP) variability represents a risk factor for MACCE after ICH, independent of average BP. Methods and Results We analyzed data from prospective ICH cohort studies at Massachusetts General Hospital and the University of Hong Kong. We captured long-term (ie, visit-to-visit) BP variability, quantified as individual participants' variation coefficient. We explored determinants of systolic and diastolic BP variability and generated survival analyses models to explore their association with MACCE. Among 1828 survivors of ICH followed for a median of 46.2 months we identified 166 with recurrent ICH, 68 with ischemic strokes, and 69 with myocardial infarction. Black (coefficient +3.8, SE 1.3) and Asian (coefficient +2.2, SE 0.4) participants displayed higher BP variability. Long-term systolic BP variability was independently associated with recurrent ICH (subhazard ratio [SHR], 1.82; 95% CI, 1.19-2.79), ischemic stroke (SHR, 1.62; 95% CI, 1.06-2.47), and myocardial infarction (SHR, 1.54; 95% CI, 1.05-2.24). Average BP during follow-up did not modify the association between long-term systolic BP variability and MACCE. Conclusions Long-term BP variability is a potent risk factor for recurrent hemorrhage, ischemic stroke, and myocardial infarction after ICH, even among survivors with well-controlled hypertension. Our findings support the hypothesis that combined control of average BP and its variability after ICH is required to minimize incidence of MACCE.
Keywords: hypertension; intracranial hemorrhage; secondary prevention.
Figures

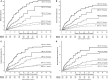


References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

