Long-term Clinical Outcomes and Prognostic Factors After Endovascular Treatment in Patients With Chronic Limb Threatening Ischemia
- PMID: 35257522
- PMCID: PMC9160641
- DOI: 10.4070/kcj.2021.0342
Long-term Clinical Outcomes and Prognostic Factors After Endovascular Treatment in Patients With Chronic Limb Threatening Ischemia
Abstract
Background and objectives: Endovascular therapy (EVT) first strategy has been widely adopted for the treatment of chronic limb threatening ischemia (CLTI) patients in real-world practice. This study aimed to investigate long-term outcomes of CLTI patients who underwent EVT and identify prognostic factors.
Methods: From the retrospective cohorts of a Korean multicenter endovascular therapy registry, 1,036 patients with CLTI (792 men, 68.8 ± 9.5 years) were included. The primary endpoint was amputation-free survival (AFS) defined as the absence of major amputation or death. Secondary endpoints were major adverse limb events (MALE; a composite of major amputation, minor amputation, and reintervention).
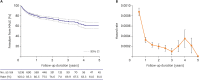
Results: Five-year AFS and freedom from MALE were 69.8% and 61%, respectively. After multivariate analysis, age (hazard ratio [HR], 1.476; p<0.001), end-stage renal disease (ESRD; HR, 2.340; p<0.001), Rutherford category (RC) 6 (HR, 1.456; p=0.036), and suboptimal EVT (HR, 1.798; p=0.005) were identified as predictors of major amputation or death, whereas smoking (HR, 0.594; p=0.007) was protective. Low body mass index (HR, 1.505; p=0.046), ESRD (HR, 1.648; p=0.001), femoropopliteal lesion (HR, 1.877; p=0.004), RC-6 (HR, 1.471; p=0.008), and suboptimal EVT (HR, 1.847; p=0.001) were predictors of MALE. The highest hazard rates were observed during the first 6 months for both major amputation or death and MALE. After that, the hazard rate decreased and rose again after 3-4 years.
Conclusions: In CLTI patients, long-term outcomes of EVT were acceptable. ESRD, RC-6, and suboptimal EVT were common predictors for poor clinical outcomes.
Trial registration: ClinicalTrials.gov Identifier: NCT02748226.
Keywords: Endovascular procedures; Peripheral arterial disease; Prognosis; Treatment outcome.
Copyright © 2022. The Korean Society of Cardiology.
Conflict of interest statement
The authors have no financial conflicts of interest.
Figures

References
-
- Farber A, Eberhardt RT. The current state of critical limb ischemia: a systematic review. JAMA Surg. 2016;151:1070–1077. - PubMed
-
- Gerhard-Herman MD, Gornik HL, Barrett C, et al. 2016 AHA/ACC guideline on the management of patients with lower extremity peripheral artery disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2017;135:e726–e779. - PMC - PubMed
-
- Aboyans V, Ricco JB, Bartelink MEL, et al. 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS): document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteriesEndorsed by: the European Stroke Organization (ESO)The Task Force for the Diagnosis and Treatment of Peripheral Arterial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS) Eur Heart J. 2018;39:763–816. - PubMed
-
- Adam DJ, Beard JD, Cleveland T, et al. Bypass versus angioplasty in severe ischaemia of the leg (BASIL): multicentre, randomised controlled trial. Lancet. 2005;366:1925–1934. - PubMed
-
- Mustapha JA, Katzen BT, Neville RF, et al. Propensity score-adjusted comparison of long-term outcomes among revascularization strategies for critical limb ischemia. Circ Cardiovasc Interv. 2019;12:e008097. - PubMed
Associated data
LinkOut - more resources
Full Text Sources
Medical

