Co-infection of SARS-CoV-2 and influenza viruses: A systematic review and meta-analysis
- PMID: 35262019
- PMCID: PMC8349735
- DOI: 10.1016/j.jcvp.2021.100036
Co-infection of SARS-CoV-2 and influenza viruses: A systematic review and meta-analysis
Abstract
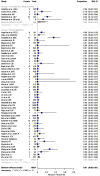
We conducted this meta-analysis to determine the proportion of co-infection with influenza viruses in SARS-CoV-2 positive patients and to investigate the severity of COVID-19 in these patients. We included studies with SARS-CoV-2 infection confirmed by qRT-PCR and influenza virus infection (A and/or B) by nucleic acid tests. The proportion of co-infection was compared between children and adults, and between critically ill or deceased patients compared to overall patients. Fifty-four articles were included. The overall proportion of co-infection was 0.7%, 95%CI = [0.4 - 1.3]. Most influenza co-infections were due to the influenza A virus (74.4%). The proportion of co-infection with influenza viruses among children (3.2%, 95% CI = [0.9 - 10.9]) was significantly higher than that in adult patients (0.3%, 95% CI = [0.1 - 1.2]), p-value <0.01. The proportion of co-infection with influenza viruses among critically ill patients tended to be higher than that in overall patients (2.2%, 95% CI = [0.3 - 22.4] versus 0.6%, 95% CI = [0.3 - 1.2], respectively, p-value = 0.22). Screening for pathogens in co-infection, particularly influenza viruses in patients infected with SARS-CoV-2, is necessary. This warrants close surveillance and investigation of the co-incidences and interactions of SARS-CoV-2 and other respiratory viruses, which is facilitated by the expansion of syndromic diagnosis approaches through the use of multiplex PCR assays.
Keywords: COVID-19; Co-infection; Influenza; Molecular; SARS-CoV-2.
© 2021 The Authors. Published by Elsevier Ltd.
Conflict of interest statement
None.
Figures
References
-
- D’Abramo A, Lepore L, Palazzolo C, Barreca F, Liuzzi G, Lalle E, et al. Acute respiratory distress syndrome due to SARS-CoV-2 and Influenza A co-infection in an Italian patient: mini-review of the literature. Int. J. Infect. Dis. 2020;97:236–239. doi: 10.1016/j.ijid.2020.06.056. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous