Small Cell Lung Cancer Transformation following Treatment in EGFR-Mutated Non-Small Cell Lung Cancer
- PMID: 35268520
- PMCID: PMC8911080
- DOI: 10.3390/jcm11051429
Small Cell Lung Cancer Transformation following Treatment in EGFR-Mutated Non-Small Cell Lung Cancer
Abstract
EGFR-mutated lung adenocarcinoma patients who received tyrosine kinase inhibitors (TKIs) may initially respond to therapy, but over time, resistance eventually occurs. In a small population (5-10%), these patients can have a histological transformation to SCLC. Nine patients with EGFR-mutated lung adenocarcinoma who transformed to SCLC were evaluated at City of Hope. Patient clinical and pathology data, including multiple next-generation sequencing (NGS) results, clinical therapies, histology, and outcomes, were collected across multiple time points. Descriptive statistics were utilized to visualize and interpret the clinical therapeutic timeline and molecular transformation profiles for these patients. All patients received at least one line of EGFR TKI therapies prior to small cell lung cancer transformation, including erlotinib, afatinib, and osimertinib. Two patients also received chemotherapy prior to transformation (one with immunotherapy). The median months to small cell lung cancer transformation was 16 months, ranging from 4-49 months. The median overall survival (OS) was 29 months from diagnosis, with the minimum of 16 months and maximum of 62 months. The majority of patients had EGFR exon 19 deletion (n = 7, 77.8%), and no patients had a change of original oncogenic EGFR mutation over the different time points. Though a TP53 mutation was detected in eight patients (88.9%) either at the first biopsy or the subsequent biopsies, an RB1 alteration was only detected in one patient at presentation, and three patients upon subsequent biopsies (n = 4, 44.4%). Each patient had a unique molecular profile in the subsequent molecular testing post-transformation, but BRAF alterations occurred frequently, including BRAF rearrangement (n = 1), fusion (n = 1), and amplification (n = 1). Our results showed that EGFR-mutated lung adenocarcinoma to SCLC transformation patients have a unique histological, molecular, and clinical profile over multiple time points, with further heterogeneity that is not currently reported in the literature, and we suggest more work is required to better understand the molecular heterogeneity and clinical outcomes over time for this EGFR TKI resistance subtype.
Keywords: EGFR; NSCLC; SCLC; genomics; precision medicine; transformation.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
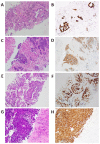


Similar articles
-
Genomic alterations and clinical outcomes in patients with lung adenocarcinoma with transformation to small cell lung cancer after treatment with EGFR tyrosine kinase inhibitors: A multicenter retrospective study.Lung Cancer. 2021 May;155:20-27. doi: 10.1016/j.lungcan.2021.03.006. Epub 2021 Mar 9. Lung Cancer. 2021. PMID: 33714778
-
Clinicopathologic and molecular characteristics of EGFR-mutant lung adenocarcinomas that transform to small cell lung cancer after TKI therapy.Transl Lung Cancer Res. 2022 Mar;11(3):452-461. doi: 10.21037/tlcr-21-665. Transl Lung Cancer Res. 2022. PMID: 35399568 Free PMC article.
-
Heterogeneous resistance mechanisms in an EGFR exon 19-mutated non-small cell lung cancer patient treated with erlotinib: Persistent FGFR3-mutation, localized transformation to EGFR-mutated SCLC, and acquired T790M EGFR-mutation.Lung Cancer. 2017 Nov;113:14-17. doi: 10.1016/j.lungcan.2017.08.024. Epub 2017 Sep 1. Lung Cancer. 2017. PMID: 29110841
-
Outcomes in Patients With Lung Adenocarcinoma With Transformation to Small Cell Lung Cancer After EGFR Tyrosine Kinase Inhibitors Resistance: A Systematic Review and Pooled Analysis.Front Oncol. 2022 Jan 28;11:766148. doi: 10.3389/fonc.2021.766148. eCollection 2021. Front Oncol. 2022. PMID: 35223450 Free PMC article.
-
Ideal sequencing in Stage IV epidermal growth factor receptor mutant Non-Small-Cell Lung Cancer.Indian J Cancer. 2022 Mar;59(Supplement):S80-S89. doi: 10.4103/ijc.IJC_50_21. Indian J Cancer. 2022. PMID: 35343193 Review.
Cited by
-
Clinical Network Systems Biology: Traversing the Cancer Multiverse.J Clin Med. 2023 Jul 7;12(13):4535. doi: 10.3390/jcm12134535. J Clin Med. 2023. PMID: 37445570 Free PMC article. Review.
-
Histomorphological transformation from non-small cell lung carcinoma to small cell lung carcinoma after targeted therapy or immunotherapy: A report of two cases.Front Oncol. 2022 Nov 9;12:1022705. doi: 10.3389/fonc.2022.1022705. eCollection 2022. Front Oncol. 2022. PMID: 36439460 Free PMC article.
-
Current and Emerging Treatment Options for Patients with Metastatic EGFR-Mutated Non-small Cell Lung Cancer After Progression on Osimertinib and Platinum-Based Chemotherapy: A Podcast Discussion.Adv Ther. 2023 Dec;40(12):5579-5590. doi: 10.1007/s12325-023-02680-1. Epub 2023 Oct 6. Adv Ther. 2023. PMID: 37801233 Free PMC article.
-
Immunological biomarkers and gene signatures predictive of radiotherapy resistance in non-small cell lung cancer.Front Immunol. 2025 May 29;16:1574113. doi: 10.3389/fimmu.2025.1574113. eCollection 2025. Front Immunol. 2025. PMID: 40510341 Free PMC article.
-
Making the Best Use of Available Weapons for the Inevitable Rivalry-Resistance to EGFR-TKIs.Biomedicines. 2023 Apr 10;11(4):1141. doi: 10.3390/biomedicines11041141. Biomedicines. 2023. PMID: 37189759 Free PMC article. Review.
References
-
- John T., Akamatsu H., Delmonte A., Su W.C., Lee J.S., Chang G.C., Huang X., Jenkins S., Wu Y.L. EGFR mutation analysis for prospective patient selection in AURA3 phase III trial of osimertinib versus platinum-pemetrexed in patients with EGFR T790M-positive advanced non-small-cell lung cancer. Lung Cancer. 2018;126:133–138. doi: 10.1016/j.lungcan.2018.10.027. - DOI - PubMed
-
- Marcoux N., Gettinger S.N., O’Kane G., Arbour K.C., Neal J.W., Husain H., Evans T.L., Brahmer J.R., Muzikansky A., Bonomi P.D., et al. EGFR-Mutant Adenocarcinomas That Transform to Small-Cell Lung Cancer and Other Neuroendocrine Carcinomas: Clinical Outcomes. J. Clin. Oncol. 2019;37:278–285. doi: 10.1200/JCO.18.01585. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

