Perioperative platelet count in peripheral blood is associated with the early stage of PND after major orthopedic surgery: a prospective observational study
- PMID: 35287583
- PMCID: PMC8919528
- DOI: 10.1186/s12877-022-02899-7
Perioperative platelet count in peripheral blood is associated with the early stage of PND after major orthopedic surgery: a prospective observational study
Abstract
Background: Perioperative neurocognitive disorders (PND) are common complications of major surgery among elderly patients, remarkably decreasing patients' life quality. Platelet count has been proved to be an essential factor in inflammation. However, as far as we know, the relationship between platelet count and PND is not clear yet in the orthopedic area. PND could be a long-term disease, which sometimes lasts for several years, and it is meaningful to find a biomarker of PND at the early stage. Thus, we designed this study to find out the association between perioperative platelet count and occurrence of PND, and determine whether preoperative platelet count could be a biomarker of the early stage of PND.
Methods: A prospective observational study was performed on the patients who would take total knee arthroplasty or total hip arthroplasty. Their peripheral platelets were counted by blood routine examination 1 day before and 3 days after the surgery. And we assessed their neurocognitive functions 1 day before and 3 days after the surgery. These data were recorded and analyzed to find out the relationship between platelet count and the occurrence of PND.
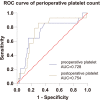
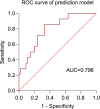
Results: Eventually, 70 patients finished the whole process, and 14 of them developed PND. The median preoperative platelet count in the PND group was significantly higher than that in the non-PND group (239 vs 168 × 10^9/L, p = 0.009). Preoperative platelet count was an independent risk factor for PND (odds ratio = 1.014, 95% confidence interval [CI] 1.000-1.027, P = 0.043) in the logistic multivariable regression, while the area under the curve of the receiver operating characteristic curve of the prediction model was 0.796 (95% CI 0.676-0.916).
Conclusions: The higher preoperative and postoperative level of platelet count in the peripheral blood were associated with the early stage of PND, and preoperative platelet count could be a potential predictor of the early stage of PND in patients undergoing major orthopedic surgeries.
Trial registration: Chinese Clinical Trial Registry: ChiCTR2000033001 , registration date: 17 May 2020.
Keywords: Biomarker; Elderly major orthopedic surgery; Perioperative neurocognitive disorders; Perioperative platelet count.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Correlation between heart rate variability and perioperative neurocognitive disorders in patients undergoing non-cardiac surgery: A retrospective cohort study.PLoS One. 2024 Apr 2;19(4):e0297337. doi: 10.1371/journal.pone.0297337. eCollection 2024. PLoS One. 2024. PMID: 38564647 Free PMC article.
-
Decreased brain-derived neurotrophic factor levels may predict early perioperative neurocognitive disorder in patients undergoing coronary artery bypass surgery: A prospective observational pilot study.J Clin Anesth. 2021 Aug;71:110235. doi: 10.1016/j.jclinane.2021.110235. Epub 2021 Mar 25. J Clin Anesth. 2021. PMID: 33774438
-
Perioperative neurocognitive disorder changes in elderly diabetes patients within 30 days after surgery: a retrospective cohort study.Aging Clin Exp Res. 2023 Dec;35(12):2911-2918. doi: 10.1007/s40520-023-02583-9. Epub 2023 Oct 17. Aging Clin Exp Res. 2023. PMID: 37847351
-
The impact of frailty as a critical mediator causing postoperative neurocognitive disorders in postoperative cardiac patients.Curr Probl Cardiol. 2024 May;49(5):102528. doi: 10.1016/j.cpcardiol.2024.102528. Epub 2024 Mar 16. Curr Probl Cardiol. 2024. PMID: 38492615 Review.
-
Proposing Bromo-epi-androsterone (BEA) for perioperative neurocognitive disorders with Interleukin-6 as a druggable target.J Clin Anesth. 2025 Feb;101:111736. doi: 10.1016/j.jclinane.2024.111736. Epub 2025 Jan 1. J Clin Anesth. 2025. PMID: 39746239 Review.
Cited by
-
Association between cerebrovascular disease and perioperative neurocognitive disorders: a retrospective cohort study.Int J Surg. 2024 Jan 1;110(1):353-360. doi: 10.1097/JS9.0000000000000842. Int J Surg. 2024. PMID: 37916928 Free PMC article.
-
D-Dimer/Platelet Ratio Predicts in-Hospital Death in Patients with Acute Type a Aortic Dissection.Int J Gen Med. 2024 Nov 11;17:5191-5202. doi: 10.2147/IJGM.S490858. eCollection 2024. Int J Gen Med. 2024. PMID: 39554871 Free PMC article.
-
Development and validation comparison of multiple models for perioperative neurocognitive disorders during hip arthroplasty.Sci Rep. 2025 Mar 19;15(1):9393. doi: 10.1038/s41598-025-93324-7. Sci Rep. 2025. PMID: 40102571 Free PMC article.
-
The health-related quality of life for hemiarthroplasty and total hip arthroplasty in the elderly: A meta-analysis.Front Med (Lausanne). 2023 Feb 24;10:1022584. doi: 10.3389/fmed.2023.1022584. eCollection 2023. Front Med (Lausanne). 2023. PMID: 36910484 Free PMC article.
-
Peripheral blood mononuclear cell transcriptomic trajectories reveal dynamic regulation of inflammatory actors in delirium.medRxiv [Preprint]. 2025 Feb 20:2025.02.14.25322163. doi: 10.1101/2025.02.14.25322163. medRxiv. 2025. PMID: 40034792 Free PMC article. Preprint.
References
-
- Caza N, Taha R, Qi Y, Blaise G. The effects of surgery and anesthesia on memory and cognition. Prog Brain Res. 2008;169:409–422. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

