Challenges in the management of bilateral eyelid closure in Stevens-Johnson Syndrome
- PMID: 35308589
- PMCID: PMC8924635
- DOI: 10.1016/j.ajoc.2022.101473
Challenges in the management of bilateral eyelid closure in Stevens-Johnson Syndrome
Abstract
Purpose: To describe the challenges of surgically treating Stevens-Johnson syndrome (SJS) cases with bilateral eyelid closure, a serious ocular sequela.
Observations: This study involved two 69-year-old females, with subacute-stage SJS (Case 1 and Case 2), and a 37-year-old male with chronic-stage SJS (Case 3). Case 1 had undergone simultaneous bilateral symblepharon lysis at 4-months post SJS onset, and her logarithm of the minimum angle of resolution (logMAR) best-corrected visual acuity (VA) (BCVA) improved from 2.8 (both eyes) to 0.7 OD and 0.4 OS. Cases 2 and 3 underwent symblepharon lysis with intraoperative use of mitomycin C (MMC) and amniotic membrane transplantation (AMT) at 9 months (OD) and 11 months (OS) (Case 2) and at 31 years (OD) (Case 3) post SJS onset. At 3-months postoperative, Case 3 underwent cultivated oral mucosal epithelial sheet transplantation (COMET). In both cases, BCVA (logMAR) improved with the postoperative use of limbal-rigid contact lenses (CLs); i.e., from 2.8 to 0.5 OD and 1.2 OS (Case 2) and from 2.8 to 1.1 OD (Case 3). In all 5 treated eyes, eyelid opening and VA were maintained through final follow-up.
Conclusion and importance: In severe bilateral symblepharon cases, it can be difficult to predict postoperative outcomes, as proper surgical treatment is often delayed. In SJS cases with bilateral eyelid closure, the surgical intervention strategy of AMT and COMET, combined with limbal-rigid CL wear post surgery, can result in improved vision, and symblepharon surgery might be easier and possibly result in a better prognosis when performed at the early phase.
Keywords: Amniotic membrane transplantation (AMT); Cultivated oral mucosal epithelial sheet transplantation (COMET); Improvement of visual acuity; Severe symblepharon.
© 2022 Published by Elsevier Inc.
Conflict of interest statement
The following authors have no financial disclosures: YA, KH, MU, HF, SK, CS.
Figures

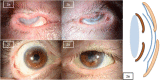

References
-
- Schwartz R.A., McDonough P.H., Lee B.W. Toxic epidermal necrolysis: part I. introduction, history, classification, clinical features, systemic manifestations, etiology, and immunopathogenesis. J Am Acad Dermatol. 2013;69(2):173. e1-13;quiz 85-86. - PubMed
-
- Bastuji-Garin S., Rzany B., Stern R.S., Shear N.H., Naldi L., Roujeau J.-C. Clinical classification of cases of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme. Arch Dermatol. 1993;129(1):92–96. - PubMed
-
- Jain R., Sharma N., Basu S., et al. Stevens-Johnson syndrome: the role of an ophthalmologist. Surv Ophthalmol. 2016;61(4):369–399. - PubMed
-
- Kohanim S., Palioura S., Saeed H.N., et al. Acute and chronic ophthalmic involvement in Stevens-Johnson syndrome/toxic epidermal necrolysis – comprehensive review and guide to therapy. II. Ophthalmic disease. Ocul Surf. 2016;14(20):168–188. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

