Endoscopic resection of superficial non-ampullary duodenal epithelial tumor
- PMID: 35310765
- PMCID: PMC8828234
- DOI: 10.1002/deo2.54
Endoscopic resection of superficial non-ampullary duodenal epithelial tumor
Abstract
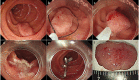
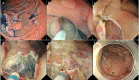
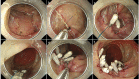
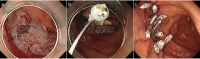
Although superficial non-ampullary duodenal epithelial tumor (SNADET) was previously considered a rare disease, in recent years, the opportunities to detect and treat SNADET are increasing. Considering the high morbidity of pancreatoduodenectomy, endoscopic resection can be a treatment option that preserves the organs and contributes maintain patients' quality of life. Endoscopic mucosal resection (EMR) is a standard treatment for relatively small lesions in gastrointestinal tracts, however, it is difficult because submucosal fibrosis frequently occurs due to the previous biopsy. Recently, some modified EMR techniques including underwater EMR (UEMR) and cold polypectomy (CP) have been proposed. In UEMR, the duodenal lumen is filled with water or saline and resected the targe lesion with a snare without injection into the submucosa. It would be a treatment option that could reduce candidates for ESD especially SNADET less than 20 mm. CP was reported as a safe and convenient means for SNADET. It would also be one of the standard treatments for diminutive lesions, though there remain some concerns on its resectability. ESD for SNADET is technically challenging, especially with an extremely high risk of adverse event (AE) with a reported bleeding rate of more than 20% and perforation rate up to about 40%. However, modified treatment techniques including the water pressure method and pocket creation method have been reported to potentially contribute to improving outcomes of ESD. Moreover, accumulated evidence shows closing the mucosal defect significantly reduces delayed adverse events after duodenal endoscopic treatments. Further studies are warranted to elucidate curative criteria, long-term outcomes, and appropriate surveillance strategy.
Keywords: duodenum; endoscopic resection; outcomes.
© 2021 The Authors. DEN Open published by John Wiley & Sons Australia, Ltd on behalf of Japan Gastroenterological Endoscopy Society.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures


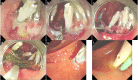
References
-
- Burgerman A, Baggenstoss AH, Cain JC. Primary malignant neoplasms of the duodenum, exclusing the papilla of vater; a clinicopathologic study of 31 cases. Gastroenterology 1956; 30: 421–31. - PubMed
-
- Barclay TH, Kent HP. Primary carcinoma of the duodenum. Gastroenterology 1956; 30: 432–46. - PubMed
-
- Arai T, Murata T, Sawabe M, Takubo K, Esaki Y. Primary adenocarcinoma of the duodenum in the elderly: Clinicopathological and immunohistochemical study of 17 cases. Pathol Int 1999; 49: 23–9. - PubMed
-
- Fischer HP, Zhou H. Pathogenesis of carcinoma of the papilla of Vater. J Hepatobiliary Pancreat Surg 2004; 11: 301–9. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous
