Laparoscopic posterior rectopexy for complete rectal prolapse: Is it the ideal procedure for males?
- PMID: 35313438
- PMCID: PMC8973478
- DOI: 10.4103/jmas.JMAS_323_20
Laparoscopic posterior rectopexy for complete rectal prolapse: Is it the ideal procedure for males?
Abstract
Background: Rectal prolapse is more common in elderly women worldwide, but in India, it predominantly occurs in young- and middle-aged males. While ventral mesh rectopexy is proposed as the preferred procedure in females, the debate on the best procedure in men is still wide open.
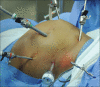
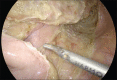
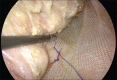
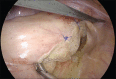
Methods: A retrospective review of all adult male patients operated for external rectal prolapse (ERP) between January 2005 and December 2019 was performed. Patients either underwent modified laparoscopic posterior mesh rectopexy (LPMR) or laparoscopic resection rectopexy (LRR). The outcome was analysed in terms of recurrence, post-operative constipation, sexual dysfunction and other complications.
Results: A total of 118 male patients were included (LPMR: 106, LRR: 12). The mean age was 46.2 years (standard deviation [SD] 11.8, range: 21-88). The mean operating time was 108 min (SD: 24). The mean length of hospital stay was 4.8 days (SD: 1.4, range: 3-11 days). There was no anastomotic leak in the LRR group. Other complications included wound infection (n = 2), mesh infection with sigmoid colon perforation (n = 1), constipation (n = 4), sexual dysfunction (n = 2), urinary urgency (n = 3) and retention of urine (n = 4). There was no mortality in both the groups. During a mean follow-up of 5.2 years, recurrent ERP was noted in one patient and partial mucosal prolapse was seen in three patients.
Conclusion: LPMR/LRR is a safe and effective treatment for ERP in men with very low recurrence rates. Randomised trials comparing modified LPMR with LVMR are needed to establish the better procedure in males.
Keywords: Males; posterior mesh rectopexy; rectal prolapse; rectopexy.
Conflict of interest statement
None
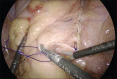
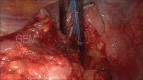
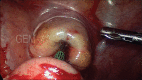
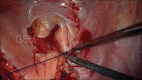
Figures
Similar articles
-
Laparoscopic ventral rectopexy using biologic mesh for the treatment of obstructed defaecation syndrome and/or faecal incontinence in patients with internal rectal prolapse: a critical appraisal of the first 100 cases.Tech Coloproctol. 2015 Apr;19(4):209-19. doi: 10.1007/s10151-014-1255-4. Epub 2015 Jan 11. Tech Coloproctol. 2015. PMID: 25577276
-
Laparoscopic ventral rectopexy for external rectal prolapse improves constipation and avoids de novo constipation.Colorectal Dis. 2010 Jun;12(6):526-32. doi: 10.1111/j.1463-1318.2009.01859.x. Epub 2009 Apr 10. Colorectal Dis. 2010. PMID: 19486104
-
Laparoscopic ventral rectopexy in male patients with external rectal prolapse is associated with a high reoperation rate.Tech Coloproctol. 2016 Oct;20(10):715-20. doi: 10.1007/s10151-016-1528-1. Epub 2016 Sep 19. Tech Coloproctol. 2016. PMID: 27641548
-
Outcome of laparoscopic ventral mesh rectopexy for full-thickness external rectal prolapse: a systematic review, meta-analysis, and meta-regression analysis of the predictors for recurrence.Surg Endosc. 2019 Aug;33(8):2444-2455. doi: 10.1007/s00464-019-06803-0. Epub 2019 Apr 30. Surg Endosc. 2019. PMID: 31041515
-
Meta-analysis of laparoscopic mesh rectopexy versus posterior sutured rectopexy for management of complete rectal prolapse.Int J Colorectal Dis. 2021 Jul;36(7):1357-1366. doi: 10.1007/s00384-021-03883-0. Epub 2021 Feb 23. Int J Colorectal Dis. 2021. PMID: 33624175 Review.
Cited by
-
Mesh Rectopexy or Resection Rectopexy for Rectal Prolapse; Is There a Gold Standard Method: A Systematic Review, Meta-Analysis and Trial Sequential Analysis.J Clin Med. 2024 Feb 28;13(5):1363. doi: 10.3390/jcm13051363. J Clin Med. 2024. PMID: 38592257 Free PMC article. Review.
-
Comparative study of laparoscopic ventral mesh rectopexy versus perineal stapler resection for external full-thickness rectal prolapse in elderly patients: enhanced outcomes and reduced recurrence rates-a retrospective cohort study.Tech Coloproctol. 2024 Apr 15;28(1):48. doi: 10.1007/s10151-024-02919-1. Tech Coloproctol. 2024. PMID: 38619626 Free PMC article.
-
Colonoscopy-assisted percutaneous sigmoidopexy (CAPS) for complete rectal prolapse treatment: Case series.Endosc Int Open. 2023 Oct 9;11(10):E931-E934. doi: 10.1055/a-2131-5037. eCollection 2023 Oct. Endosc Int Open. 2023. PMID: 37818456 Free PMC article.
-
First time use of trans-anal endorectal pull through (Soave procedure) for management of recurrent rectal mucosal prolapse in children not responding to the conventional sclerotherapy interventions: A case series.Int J Surg Case Rep. 2025 Apr;129:111176. doi: 10.1016/j.ijscr.2025.111176. Epub 2025 Mar 17. Int J Surg Case Rep. 2025. PMID: 40120326 Free PMC article.
-
Systematic literature review and meta-analysis of surgical treatment of complete rectal prolapse in male patients.Tech Coloproctol. 2024 Nov 13;28(1):158. doi: 10.1007/s10151-024-03039-6. Tech Coloproctol. 2024. PMID: 39538028
References
-
- Lundby L, Laurberg S. Laparoscopic ventral mesh rectopexy for obstructed defaecation syndrome: Time for a critical appraisal. Colorectal Dis. 2015;17:102–3. - PubMed
-
- Senapati A, Gray RG, Middleton LJ, Harding J, Hills RK, Armitage NC, et al. PROSPER: A randomised comparison of surgical treatments for rectal prolapse. Colorectal Dis. 2013;15:858–68. - PubMed
-
- Samaranayake CB, Luo C, Plank AW, Merrie AE, Plank LD, Bissett IP. Systematic review on ventral rectopexy for rectal prolapse and intussusception. Colorectal Dis. 2010;12:504–12. - PubMed
-
- D’Hoore A, Cadoni R, Penninckx F. Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg. 2004;91:1500–5. - PubMed
LinkOut - more resources
Full Text Sources

