High fibrinogen-to-albumin ratio with type 2 diabetes mellitus is associated with poor prognosis in patients undergoing percutaneous coronary intervention: 5-year findings from a large cohort
- PMID: 35313877
- PMCID: PMC8939137
- DOI: 10.1186/s12933-022-01477-w
High fibrinogen-to-albumin ratio with type 2 diabetes mellitus is associated with poor prognosis in patients undergoing percutaneous coronary intervention: 5-year findings from a large cohort
Abstract
Background: Inflammation plays a crucial role in coronary atherosclerosis progression, and growing evidence has demonstrated that the fibrinogen-to-albumin ratio (FAR), as a novel inflammation biomarker, is associated with the severity of coronary artery disease (CAD). However, the long-term risk of cardiovascular events remains indistinct in patients with different level of FAR and different glycemic metabolism status. This study was to assess 5-year clinical outcomes of diabetic and non-diabetic patients who underwent percutaneous coronary intervention (PCI) with different level of FAR.
Methods: We consecutively enrolled 10,724 patients with CAD hospitalized for PCI and followed up for the major adverse cardiac and cerebrovascular events (MACCE) covering all-cause mortality, cardiac mortality, non-fatal myocardial infarction, non-fatal ischemic stroke, and unplanned coronary revascularization. FAR was computed using the following formula: Fibrinogen (g/L)/Albumin (g/L). According to the optimal cut-off value of FAR for MACCE prediction, patients were divided into higher level of FAR (FAR-H) and lower level of FAR (FAR-L) subgroups, and were further categorized into four groups as FAR-H with DM and non-DM, and FAR-L with DM and non-DM.
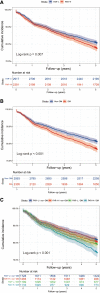
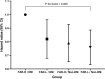
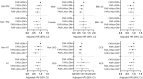
Results: 5298 patients (58.36 ± 10.36 years, 77.7% male) were ultimately enrolled in the present study. A total of 1099 (20.7%) MACCEs were documented during the 5-year follow-up. The optimal cut-off value of FAR was 0.0783 by the surv_cutpoint function. Compared to ones with FAR-H and DM, patients with FAR-L and non-DM, FAR-H and non-DM, FAR-L and DM had decreased risk of MACCEs [adjusted hazard ratio (HR): 0.75, 95% confidence interval (CI) 0.64-0.89, P = 0.001; HR: 0.78, 95% CI 0.66-0.93, P = 0.006; HR: 0.81, 95% CI 0.68-0.97, P = 0.019; respectively]. Notably, non-diabetic patients with lower level of FAR also had lower all-cause mortality and cardiac mortality risk than those in the FAR-H/DM group (HR: 0.41, 95% CI 0.27-0.63, P < 0.001; HR: 0.30, 95% CI 0.17-0.53, P < 0.001; respectively). Multivariate Cox proportional hazards regression analysis also indicated the highest risk of MACCEs in patients with FAR-H and DM than others (P for trend = 0.005). In addition, post-hoc analysis revealed consistent effects on 5-year MACCE across various subgroups.
Conclusion: In this real-world cohort study, higher level of FAR combined with DM was associated with worse 5-year outcomes among patients with CAD undergoing PCI. The level of FAR may help to identify high-risk individuals in this specific population, where more precise risk assessment should be performed.
Keywords: Fibrinogen‑to‑albumin ratio; Percutaneous coronary intervention; Prognosis; Type 2 diabetes mellitus.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures

References
-
- Sharif S, Van der Graaf Y, Cramer MJ, Kapelle LJ, de Borst GJ, Visseren FLJ, Westerink J. Low-grade inflammation as a risk factor for cardiovascular events and all-cause mortality in patients with type 2 diabetes. Cardiovasc Diabetol. 2021;20(1):220. doi: 10.1186/s12933-021-01409-0. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- Grant No. 81900323/National Natural Science Foundation of China
- No. 81770365/National Natural Science Foundation of China
- 2016YFC1301300 and 2016YFC1301301/the Ministry of Science and Technology of the People's Republic of China
- Grant No.NCRC2020013/National Clinical Research Center for Cardiovascular Diseases, Fuwai Hospital, Chinese Academy of Medical SciencesGrant
- 2020-I2M-C&T-B-049/the CAMS Innovation Fund for Medical Sciences (CIFMS)
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

