Impact of My Dose Coach App Frequency of Use on Clinical Outcomes in Type 2 Diabetes
- PMID: 35316509
- PMCID: PMC8938735
- DOI: 10.1007/s13300-022-01245-9
Impact of My Dose Coach App Frequency of Use on Clinical Outcomes in Type 2 Diabetes
Abstract
Introduction: My Dose Coach (MDC) is a US Food and Drug Administration-approved digital smartphone application designed to help users with type 2 diabetes (T2D) titrate their basal insulin (BI) according to a clinician-prescribed individualized titration plan. The aim of this analysis was to assess the impact of the frequency of MDC use on clinical outcomes.
Methods: This retrospective observational analysis included people with T2D who were registered for MDC (August 1st, 2018-April 30th, 2020) and received BI. Users with an activated care plan and ≥2 fasting blood glucose (FBG) observations spanning ≥2 weeks were defined as active. Outcomes included percentage achieving their individual FBG target, time to FBG target, change in FBG, change in insulin dose and hypoglycemia. Users were stratified into high (>3 days per week), moderate (>1- ≤3 days per week), and low (≤1 day per week) MDC usage groups.
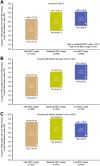
Results: The analysis included 2517 active MDC users. Approximately 49% of users had high MDC usage. Overall, 44% of users across all usage frequencies achieved their individual FBG target. High MDC use was associated with significantly better FBG target achievement and less time to FBG target versus moderate- and low-usage groups (p≤0.01 for all). Insulin dose change was significantly greater in the high- versus moderate-usage group (p=0.01). There was no significant difference in hypoglycemia incidence among MDC usage groups (12%-16% of users in any usage group).
Conclusions: More frequent MDC usage was associated with better FBG outcomes without increased hypoglycemia risk.
Keywords: Glycemic control; Mobile application; Self-management; Type 2 diabetes mellitus.
© 2022. The Author(s).
Figures



Similar articles
-
Real-World Effectiveness of My Dose Coach™-Assisted Basal Insulin Titration in People with Type 2 Diabetes in Saudi Arabia and Kuwait.Diabetes Ther. 2025 Jul 21. doi: 10.1007/s13300-025-01772-1. Online ahead of print. Diabetes Ther. 2025. PMID: 40690110
-
The Effectiveness of an App (Insulia) in Recommending Basal Insulin Doses for French Patients With Type 2 Diabetes Mellitus: Longitudinal Observational Study.JMIR Diabetes. 2023 Mar 1;8:e44277. doi: 10.2196/44277. JMIR Diabetes. 2023. PMID: 36749650 Free PMC article.
-
Efficacy of a basal insulin dose management smartphone application for controlling fasting blood glucose in patients with type-2 diabetes mellitus: A single-centre, randomised clinical study.Clin Endocrinol (Oxf). 2023 Oct;99(4):361-369. doi: 10.1111/cen.14956. Epub 2023 Aug 1. Clin Endocrinol (Oxf). 2023. PMID: 37528510 Clinical Trial.
-
Dosing of insulin glargine in the treatment of type 2 diabetes.Clin Ther. 2007 Jun;29(6):987-99. doi: 10.1016/j.clinthera.2007.06.018. Clin Ther. 2007. PMID: 17692716 Review.
-
Repaglinide : a pharmacoeconomic review of its use in type 2 diabetes mellitus.Pharmacoeconomics. 2004;22(6):389-411. doi: 10.2165/00019053-200422060-00005. Pharmacoeconomics. 2004. PMID: 15099124 Review.
Cited by
-
Insights into the Feasibility and Acceptability of a Mobile Insulin Titration Application in Clinical Practice and Its Effects on Diabetes Outcomes.touchREV Endocrinol. 2024 Apr;20(1):52-57. doi: 10.17925/EE.2024.20.1.10. Epub 2024 Feb 29. touchREV Endocrinol. 2024. PMID: 38812671 Free PMC article.
-
Use of Voice-Based Conversational Artificial Intelligence for Basal Insulin Prescription Management Among Patients With Type 2 Diabetes: A Randomized Clinical Trial.JAMA Netw Open. 2023 Dec 1;6(12):e2340232. doi: 10.1001/jamanetworkopen.2023.40232. JAMA Netw Open. 2023. PMID: 38039007 Free PMC article. Clinical Trial.
-
Real-World Effectiveness of My Dose Coach™-Assisted Basal Insulin Titration in People with Type 2 Diabetes in Saudi Arabia and Kuwait.Diabetes Ther. 2025 Jul 21. doi: 10.1007/s13300-025-01772-1. Online ahead of print. Diabetes Ther. 2025. PMID: 40690110
-
Expert Opinion on Optimizing Suboptimal Basal Insulin Titration in India: Addressing Challenges and Leveraging Digital Solutions.Diabetes Ther. 2025 Jul;16(7):1327-1339. doi: 10.1007/s13300-025-01747-2. Epub 2025 May 20. Diabetes Ther. 2025. PMID: 40392519 Free PMC article.
-
U-shaped association between online information exchange and app usage frequency: a large-scale survey of China 's online young and middle-aged people with pre diabetes and diabetes.Front Endocrinol (Lausanne). 2023 Apr 21;14:1141645. doi: 10.3389/fendo.2023.1141645. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 37152927 Free PMC article.
References
-
- American Diabetes Association. 6. Glycemic Targets: Standards of Medical Care in Diabetes-2021. Diabetes Care. 2021;44:S73–S84. - PubMed
-
- International Diabetes Federation. IDF Diabetes Atlas, Ninth edition. 2019. https://www.diabetesatlas.org/en/. Accessed 19 May 2021
LinkOut - more resources
Full Text Sources
Miscellaneous

