Femoroacetabular offset restoration in total hip arthroplasty; Digital templating a short stem vs a conventional stem
- PMID: 35317405
- PMCID: PMC8891660
- DOI: 10.5312/wjo.v13.i2.139
Femoroacetabular offset restoration in total hip arthroplasty; Digital templating a short stem vs a conventional stem
Abstract
Background: Failure in restoring individual anatomy could be a reason for persistent functional limitations post total hip arthroplasty. Femoroacetabular offset (FAO) plays an important role in anatomic restoration, as loss of offset ≥ 5 mm is associated with altered gait and decreased functional outcome. Preoperative assessment by use of digital templating has shown to be a reliable method for sizing the components in total hip arthroplasty, and can show if anatomic restoration is achieved. In recent years, short stems are growing in popularity as it could allow better restoration due to more variety in placement.
Aim: To assess whether restoration of the FAO differs between a short or a conventional stem by use of digital templating. Additionally, association of the preoperative offset and caput-colllum-diaphyseal angle (CCD-angle) within restoration of both stems was investigated, and the reliability of measurements was assessed.
Methods: A total of 100 standardized hip radiographs were used for digital templating. Restoration of FAO was classified into "restored" or "not restored", when a < 5 mm or ≥ 5 mm difference from baseline value presented, respectively. Differences between the two stems concerning proportions of correct restoration of the FAO were analyzed by use of McNemar tests. To assess association between CCD-angle and preoperative FAO with absolute FAO restoration, multi-level analysis was performed by use of a linear mixed model to account for paired measurements. Through determination of the optimal point under the curve in operating curve-analysis, bootstrapping of thousand sets was performed to determine the optimal cutoff point of the preoperative FAO for restoration within the limits of 5 mm. Three observers participated for inter-observer reliability, with two observers measuring the radiographs twice for intra-observer reliability.
Results: The mean preoperative FAO was 79.7 mm (range 62.5-113 mm), with a mean CCD-angle of 128.6° (range 114.5°-145°). The conventional stem could only restore the FAO in 72 of the cases, whereas the short stem restored the FAO in all cases. CCD-angle was not a predictor, but the preoperative FAO was. A cut-off point of 81.25 mm (95% confidence interval of 80.75-84.75 mm) in preoperative FAO was found where the conventional stem was unable to restore the FAO. Reliability of measurements was excellent, with an intra-observer reliability of 0.99 and inter-observer reliability in baseline measurements higher than 0.9 between the three observers.
Conclusion: In preoperative planning of FAO restoration in total hip arthroplasty, digital templating shows that short stems with a curve following the medial calcar are potentially better at restoring the FAO compared to conventional stems if the preoperative offset is ≥ 80.0 mm.
Keywords: Anatomic offset restoration; Conventional hip stem; Offset; Short hip stem; Total hip arthroplasty.
©The Author(s) 2022. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: There are no conflict of interest from any of the authors regarding this paper.
Figures
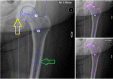


Similar articles
-
Preoperative digital planning versus postoperative outcomes in total hip arthroplasty using a calcar-guided short stem: frequent valgization can be avoided.Eur J Orthop Surg Traumatol. 2017 Jul;27(5):643-651. doi: 10.1007/s00590-017-1948-2. Epub 2017 Apr 8. Eur J Orthop Surg Traumatol. 2017. PMID: 28391517
-
Digital templating for the implantation of a curved short hip stem with an anterolateral MIS approach shows gender differences in digital templating.Arch Orthop Trauma Surg. 2022 Jul;142(7):1661-1668. doi: 10.1007/s00402-021-04005-9. Epub 2021 Jun 24. Arch Orthop Trauma Surg. 2022. PMID: 34169356 Free PMC article.
-
Validation of CT-Based Three-Dimensional Preoperative Planning in Comparison with Acetate Templating for Primary Total Hip Arthroplasty.Orthop Surg. 2022 Jun;14(6):1152-1160. doi: 10.1111/os.13298. Epub 2022 May 7. Orthop Surg. 2022. PMID: 35524643 Free PMC article.
-
Femoral offset: anatomical concept, definition, assessment, implications for preoperative templating and hip arthroplasty.Orthop Traumatol Surg Res. 2009 May;95(3):210-9. doi: 10.1016/j.otsr.2009.03.010. Epub 2009 May 6. Orthop Traumatol Surg Res. 2009. PMID: 19423418 Review.
-
The accuracy and reliability of preoperative digital 2D templating in prosthesis size prediction in uncemented versus cemented total hip arthroplasty: a systematic review and meta-analysis.EFORT Open Rev. 2021 Nov 19;6(11):1020-1039. doi: 10.1302/2058-5241.6.210048. eCollection 2021 Nov. EFORT Open Rev. 2021. PMID: 34909222 Free PMC article. Review.
Cited by
-
Offset restoration in total hip arthroplasty: Important: A current review.World J Orthop. 2024 Aug 18;15(8):696-703. doi: 10.5312/wjo.v15.i8.696. eCollection 2024 Aug 18. World J Orthop. 2024. PMID: 39165871 Free PMC article.
-
Smartphone-based digital templating using presentation software enhances accuracy in equalizing leg length and femoral offset during bipolar hemiarthroplasty for femoral neck fracture.Arch Orthop Trauma Surg. 2025 Jul 15;145(1):374. doi: 10.1007/s00402-025-05976-9. Arch Orthop Trauma Surg. 2025. PMID: 40665099
References
-
- Judge A, Cooper C, Williams S, Dreinhoefer K, Dieppe P. Patient-reported outcomes one year after primary hip replacement in a European Collaborative Cohort. Arthritis Care Res (Hoboken) 2010;62:480–488. - PubMed
-
- Hawker GA, Badley EM, Borkhoff CM, Croxford R, Davis AM, Dunn S, Gignac MA, Jaglal SB, Kreder HJ, Sale JE. Which patients are most likely to benefit from total joint arthroplasty? Arthritis Rheum. 2013;65:1243–1252. - PubMed
-
- Amlie E, Havelin LI, Furnes O, Baste V, Nordsletten L, Hovik O, Dimmen S. Worse patient-reported outcome after lateral approach than after anterior and posterolateral approach in primary hip arthroplasty. A cross-sectional questionnaire study of 1,476 patients 1-3 years after surgery. Acta Orthop. 2014;85:463–469. - PMC - PubMed
LinkOut - more resources
Full Text Sources

