Disparities in healthcare expenditures according to economic status in cancer patients undergoing end-of-life care
- PMID: 35317774
- PMCID: PMC8939210
- DOI: 10.1186/s12885-022-09373-y
Disparities in healthcare expenditures according to economic status in cancer patients undergoing end-of-life care
Abstract
Backgrounds: A desire for better outcome influences cancer patients' willingness to pay. Whilst cancer-related costs are known to have a u-shaped distribution, the actual level of healthcare utilized by patients may vary depending on income and ability to pay. This study examined patterns of healthcare expenditures in the last year of life in patients with gastric, colorectal, lung, and liver cancer and analyzed whether differences exist in the level of end-of-life costs for cancer care according to economic status.
Methods: This study is a retrospective cohort study which used data from the Korean National Elderly Sampled Cohort, 2002 to 2015. End-of-life was defined as 1 year before death. Economic status was classified into three categorical variables according to the level of insurance premium (quantiles). The relationship between the dependent and independent variables were analyzed using multiple gamma regression based on the generalized estimated equation (GEE) model.
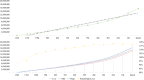
Results: This study included 3083 cancer patients, in which total healthcare expenditure was highest in the high-income group. End-of-life costs increased the most in the last 3 months of life. Compared to individuals in the 'middle' economic status group, those in the 'high' economic status group (RR 1.095, 95% CI 1.044-1.149) were likely to spend higher amounts. The percentage of individuals visiting a general hospital was highest in the 'high' economic status group, followed by the 'middle' and 'low' economic status groups.
Conclusion: Healthcare costs for cancer care increased at end-of-life in Korea. Patients of higher economic status tended to spender higher amounts of end-of-life costs for cancer care. Further in-depth studies are needed considering that end-of-life medical costs constitute a large proportion of overall expenditures. This study offers insight by showing that expenditures for cancer care tend to increase noticeably in the last 3 months of life and that differences exist in the amount spent according economic status.
Keywords: Cancer patients; Economic status; End-of-life; Healthcare disparities; Healthcare expenditure.
© 2022. The Author(s).
Conflict of interest statement
N/A
Figures
Similar articles
-
Geographical disparities in treatment and health care costs for end-of-life cancer patients in China: a retrospective study.BMC Cancer. 2019 Jan 8;19(1):39. doi: 10.1186/s12885-018-5237-1. BMC Cancer. 2019. PMID: 30621633 Free PMC article.
-
Escalating Health Care Expenditures in Cancer Decedents' Last Year of Life: A Decade of Evidence from a Retrospective Population-Based Cohort Study in Taiwan.Oncologist. 2017 Apr;22(4):460-469. doi: 10.1634/theoncologist.2016-0283. Epub 2017 Feb 23. Oncologist. 2017. PMID: 28232596 Free PMC article.
-
Association of healthcare expenditures with aggressive versus palliative care for cancer patients at the end of life: a cross-sectional study using claims data in Japan.Int J Qual Health Care. 2014 Feb;26(1):79-86. doi: 10.1093/intqhc/mzt081. Epub 2013 Nov 13. Int J Qual Health Care. 2014. PMID: 24225269
-
Relating cause of death with place of care and healthcare costs in the last year of life for patients who died from cancer, chronic obstructive pulmonary disease, heart failure and dementia: A descriptive study using registry data.Palliat Med. 2017 Apr;31(4):338-345. doi: 10.1177/0269216316685029. Epub 2017 Jan 6. Palliat Med. 2017. PMID: 28056634
-
Impact of socioeconomic status on end-of-life costs: a systematic review and meta-analysis.BMC Palliat Care. 2020 Mar 23;19(1):35. doi: 10.1186/s12904-020-0538-y. BMC Palliat Care. 2020. PMID: 32293403 Free PMC article.
Cited by
-
Days spent with healthcare contact by patients with metastatic castrate resistant prostate cancer in the last year of life.Oncologist. 2025 May 8;30(5):oyaf046. doi: 10.1093/oncolo/oyaf046. Oncologist. 2025. PMID: 40377439 Free PMC article.
-
Marginalized two part model for analyzing multilevel semicontinuous medical costs in Iranian households.Sci Rep. 2025 Mar 3;15(1):7491. doi: 10.1038/s41598-025-91309-0. Sci Rep. 2025. PMID: 40032955 Free PMC article.
-
Cancer care patterns in South Korea: Types of hospital where patients receive care and outcomes using national health insurance claims data.Cancer Med. 2023 Jul;12(13):14707-14717. doi: 10.1002/cam4.6093. Epub 2023 May 18. Cancer Med. 2023. PMID: 37199387 Free PMC article.
-
Economic Burden of Cancer for the First Five Years after Cancer Diagnosis in Patients with Human Immunodeficiency Virus in Korea.J Cancer Prev. 2023 Jun 30;28(2):53-63. doi: 10.15430/JCP.2023.28.2.53. J Cancer Prev. 2023. PMID: 37434797 Free PMC article.
-
Health expenditure trajectory and gastric cancer incidence in the National Health Insurance Senior Cohort: a nested case-control study.BMC Health Serv Res. 2024 Sep 16;24(1):1076. doi: 10.1186/s12913-024-11494-y. BMC Health Serv Res. 2024. PMID: 39285469 Free PMC article.
References
-
- OECD . Cancer care. 2013.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical