Metallosis following hip arthroplasty: two case reports
- PMID: 35317840
- PMCID: PMC8941771
- DOI: 10.1186/s13256-022-03336-4
Metallosis following hip arthroplasty: two case reports
Abstract
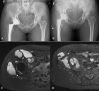
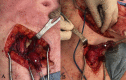
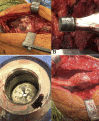
Background: There has been increasing recognition of local and systemic adverse events associated with the release of metal ions and nanoparticles from hip arthroplasty components. Adverse local tissue reactions to metal ion debris can include periprosthetic solid and cystic masses known as pseudotumors. These masses can result in pain, swelling, extensive destruction to surrounding hip soft-tissues, and compression syndromes on neurovascular, gastrointestinal, and genitourinary structures. As reports of pseudotumors requiring multidisciplinary excision are limited, we present two pseudotumor cases that were excised through a combined approach.
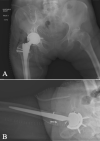
Case presentations: The first case involves a 60-year-old Caucasian female with a large pseudotumor with intrapelvic and vascular involvement associated with a metal-on-polyethylene total hip arthroplasty, excised with contributions from general surgery, vascular surgery, and orthopedic surgery. Pseudotumor excision was followed by a revision total hip reconstruction in addition to an abductor mechanism reconstruction with tendo-Achilles allograft. The second case is that of a 64-year-old Caucasian female with a pseudotumor in close relationship to the femoral vessels following a metal-on-metal hip resurfacing, excised with a combination of vascular surgery and orthopedic surgery, with subsequent revision total hip reconstruction.
Conclusions: There remains a lack of literature to support the extensiveness of pseudotumor excision required in complex cases with significant intrapelvic or vascular involvement. Given the potential for significant adverse effects of large masses, the authors' preference is to involve a multidisciplinary team to achieve a more comprehensive excision while minimizing the risk of potential complications.
Keywords: Femoral vessels; Hip resurfacing; Metallosis; Pseudotumor; Total hip arthroplasty; Vascular compression.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
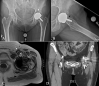
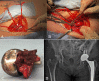
Similar articles
-
Higher Prevalence of Mixed or Solid Pseudotumors in Metal-on-Polyethylene Total Hip Arthroplasty Compared With Metal-on-Metal Total Hip Arthroplasty and Resurfacing Hip Arthroplasty.J Arthroplasty. 2018 Jul;33(7):2279-2286. doi: 10.1016/j.arth.2018.02.011. Epub 2018 Feb 12. J Arthroplasty. 2018. PMID: 29526334
-
Inflammatory pseudotumor complicating metal-on-highly cross-linked polyethylene total hip arthroplasty.J Arthroplasty. 2012 Feb;27(2):324.e5-8. doi: 10.1016/j.arth.2011.03.013. Epub 2011 Apr 16. J Arthroplasty. 2012. PMID: 21498036
-
Vascular tumor in metal-on-polyethylene THA requiring hemipelvectomy.Orthopedics. 2013 Jul;36(7):e974-7. doi: 10.3928/01477447-20130624-32. Orthopedics. 2013. PMID: 23823059
-
Metallosis after metal-on-polyethylene total hip arthroplasty.Am J Orthop (Belle Mead NJ). 2008 Feb;37(2):E18-25. Am J Orthop (Belle Mead NJ). 2008. PMID: 18401490 Review.
-
A case example and literature review of catastrophic wear before catastrophic failure: identification of trunnionosis and metallosis in metal-on-polyethylene hip arthroplasty prior to frank failure or fracture.Eur J Orthop Surg Traumatol. 2019 Apr;29(3):711-715. doi: 10.1007/s00590-018-2333-5. Epub 2018 Oct 29. Eur J Orthop Surg Traumatol. 2019. PMID: 30374642 Review.
Cited by
-
Association between metallic implants and stroke in US adults from NHANES 2015-2023 a cross-sectional study.Front Aging Neurosci. 2024 Dec 20;16:1505645. doi: 10.3389/fnagi.2024.1505645. eCollection 2024. Front Aging Neurosci. 2024. PMID: 39759400 Free PMC article.
-
Blood Metal Ion Levels After Hip Resurfacing: A Comparison of 2 Different Implants.Arthroplast Today. 2024 Oct 30;30:101555. doi: 10.1016/j.artd.2024.101555. eCollection 2024 Dec. Arthroplast Today. 2024. PMID: 39539683 Free PMC article.
-
The role of femoral head size in metal-on-metal hip arthroplasty: analysis of a cohort of 3813 patients with long term follow-up.Arch Orthop Trauma Surg. 2024 Nov;144(11):4809-4818. doi: 10.1007/s00402-024-05567-0. Epub 2024 Nov 5. Arch Orthop Trauma Surg. 2024. PMID: 39496883 Free PMC article.
-
Metallosis Following Non-Metal-on-Metal Hip Arthroplasty: A Case Report and Review.J Orthop Case Rep. 2024 Sep;14(9):111-115. doi: 10.13107/jocr.2024.v14.i09.4748. J Orthop Case Rep. 2024. PMID: 39253647 Free PMC article.
-
Are We Ready for Pseudotumors in Total Ankle Arthroplasty? A Case Report.J Clin Med. 2025 Jan 20;14(2):649. doi: 10.3390/jcm14020649. J Clin Med. 2025. PMID: 39860653 Free PMC article.
References
-
- Desai BR, Sumarriva GE, Chimento GF. Pseudotumor recurrence in a post-revision total hip arthroplasty with stem neck modularity: a case report. World J Orthop. 2020;11(2):116–22. https://www.wjgnet.com/2218-5836/full/v11/i2/116.htm. - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

