Does increasing estrogen dose during frozen embryo transfer affect pregnancy rate?
- PMID: 35322300
- PMCID: PMC9107563
- DOI: 10.1007/s10815-022-02470-8
Does increasing estrogen dose during frozen embryo transfer affect pregnancy rate?
Abstract
Objective: To assess the effect of increasing estrogen doses during hormone therapy frozen embryo transfer (HT-FET) cycles on endometrial thickness and success rates compared to patients who received fixed estrogen dose.
Materials and methods: A retrospective study from a university-based fertility clinic during the years 2008-2021. We compared two groups: the fixed-dose group (i.e., received 6 mg estradiol dose daily until embryo transfer) and the increased-dose group (i.e., the initial estradiol dose was 6 mg daily, and was increased during the cycle).
Primary outcome: clinical pregnancy rate.
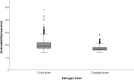
Results: The study included 5452 cycles of HT-FET: 4774 cycles in the fixed-dose group and 678 cycles in the increased-dose group. Ultrasound scan on days 2-3 of the cycle showed endometrial thickness slightly different between the two groups (4.2 mm in the fixed-dose and 4.0 mm in the increased-dose group, P = 0.003). The total estrogen dose was higher, and the treatment duration was longer in the increased than the fixed-dose group (122 mg vs. 66 mg and 17 days vs. 11 days, respectively; P < 0.001). The last ultrasound scan done before the addition of progesterone showed that the endometrial thickness was significantly thicker in the fixed than the increased-dose group (9.5 mm vs. 8.3 mm; P < 0.001). The clinical pregnancy rates were 35.8% in the increased-group vs. 34.1% in the fixed-dose group; P = 0.401.
Conclusions: The increased-dose group had thinner endometrium despite the higher doses of estrogen and longer treatment duration than the fixed-dose group. However, the pregnancy rates were similar between the two groups.
Keywords: Embryo transfer; Estrogen; Frozen embryo; IVF; Outcome; Pregnancy.
© 2022. The Author(s), under exclusive licence to Springer Science+Business Media, LLC, part of Springer Nature.
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Comparison between oral and vaginal estrogen usage in inadequate endometrial patients for frozen-thawed blastocysts transfer.Int J Clin Exp Pathol. 2014 Sep 15;7(10):6992-7. eCollection 2014. Int J Clin Exp Pathol. 2014. PMID: 25400786 Free PMC article.
-
Impact of an estrogen replacement regimen on live birth rate in frozen-thawed good-quality embryo transfer.Int J Gynaecol Obstet. 2023 Mar;160(3):829-835. doi: 10.1002/ijgo.14366. Epub 2022 Aug 15. Int J Gynaecol Obstet. 2023. PMID: 35869963
-
[The value of serum estradiol concentration on the day of endometrial transformation in predicting the outcome of frozen-thawed embryo transfer in hormone replacement cycle].Zhonghua Yu Fang Yi Xue Za Zhi. 2022 Jul 6;56(7):973-979. doi: 10.3760/cma.j.cn112150-20220214-00138. Zhonghua Yu Fang Yi Xue Za Zhi. 2022. PMID: 35899351 Chinese.
-
Endometrial preparation for women undergoing embryo transfer with frozen embryos or embryos derived from donor oocytes.Cochrane Database Syst Rev. 2020 Oct 28;10(10):CD006359. doi: 10.1002/14651858.CD006359.pub3. Cochrane Database Syst Rev. 2020. PMID: 33112418 Free PMC article.
-
Effect of estrogen exposure on pregnancy outcomes in artificial frozen-thawed embryo transfer cycles.Gynecol Endocrinol. 2024 Dec;40(1):2352142. doi: 10.1080/09513590.2024.2352142. Epub 2024 May 23. Gynecol Endocrinol. 2024. PMID: 38781518 Review.
Cited by
-
Preparation of the endometrium for frozen embryo transfer: an update on clinical practices.Reprod Biol Endocrinol. 2023 Jun 8;21(1):52. doi: 10.1186/s12958-023-01106-5. Reprod Biol Endocrinol. 2023. PMID: 37291605 Free PMC article. Review.
References
-
- European IVF-monitoring Consortium (EIM) for the European Society of Human Reproduction and Embryology (ESHRE) Wyns C, Bergh C, Calhaz-Jorge C, De Geyter C, Kupka MS, Motrenko T, Rugescu I, Smeenk J, Tandler-Schneider A, Vidakovic S, Goossens V. ART in Europe, 2016: results generated from European registries by ESHRE. Hum Reprod Open. 2020;2020(3):hoaa032. doi: 10.1093/hropen/hoaa032. - DOI - PMC - PubMed
-
- Cimadomo D, Soscia D, Vaiarelli A, Maggiulli R, Capalbo A, Ubaldi FM, Rienzi L. Looking past the appearance: a comprehensive description of the clinical contribution of poor-quality blastocysts to increase live birth rates during cycles with aneuploidy testing. Hum Reprod. 2019;34:1206–1214. doi: 10.1093/humrep/dez078. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources