Alcohol-related hepatocellular carcinoma is a heterogenous condition: Lessons from a latent class analysis
- PMID: 35324065
- PMCID: PMC9373918
- DOI: 10.1111/liv.15256
Alcohol-related hepatocellular carcinoma is a heterogenous condition: Lessons from a latent class analysis
Abstract
Background: Alcohol-associated hepatocellular carcinoma (AL-HCC) poor prognosis has been attributed to diagnosis at a later stage. However, host factors and specific health trajectories have been associated with severe outcomes in alcohol-related liver disease. We hypothesize AL-HCC is not a homogeneous condition but encompasses subgroups yielding different outcomes.
Aims: Our aim was to provide a first attempt at a clinical phenotyping of AL-HCC.
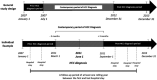
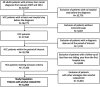
Methods: We analysed data for the calendar years 2007-2013 from the French nationwide administrative hospital database. We selected patients with AL-HCC only. Clustering of AL-HCC phenotypes was performed by latent class analysis (LCA).
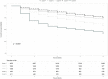
Results: The study included 11 363 patients with AL-HCC, mainly male (89.6%), median age 67 years [IQR: 61; 74] of which 71.2% had at least one metabolic comorbidity. Five phenotypes were identified. Phenotype 1 (41.4%) displayed high rates of unrecognized cirrhosis prior to HCC diagnosis (81%), low rates of metabolic comorbidities (diabetes 13%), and mostly compensated liver disease at HCC diagnosis while the four other phenotypes displayed high rates of metabolic comorbidities (diabetes up to 100%), various patterns of liver disease trajectories and overall 42% unrecognized cirrhosis. In adjusted survival analysis, compared to phenotype 1, risk of death after HCC diagnosis was significantly different for all phenotypes.
Conclusion: LCA uncovers AL-HCC is a heterogeneous condition with distinct phenotypes yielding specific survival outcomes. Frequent unrecognized cirrhosis prior to HCC underlines the urgent need for implementing strategies to identify the underlying liver disease prior to HCC onset in patients with documented alcohol use disorders and metabolic comorbidities.
Keywords: alcohol; cluster; liver cancer; survival.
© 2022 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd.
Conflict of interest statement
The authors have no conflict of interest to declare related to this study.
Figures


References
-
- Bray F, Ferlay J, Laversanne M, et al. Cancer incidence in five continents: inclusion criteria, highlights from volume X and the global status of cancer registration. Int J Cancer. 2015;137(9):2060‐2071. - PubMed
-
- Forner A, Reig M, Bruix J. Hepatocellular carcinoma. Lancet. 2018;391(10127):1301‐1314. - PubMed
-
- World Health Organization. Management of Substance Abuse Team . Global status report on alcohol and health. World Health Organization; 2018.
-
- Pimpin L, Cortez‐Pinto H, Negro F, et al. Burden of liver disease in Europe: epidemiology and analysis of risk factors to identify prevention policies. J Hepatol. 2018;69(3):718‐735. - PubMed
-
- Costentin CE, Mourad A, Lahmek P, et al. Hepatocellular carcinoma is diagnosed at a later stage in alcoholic patients: results of a prospective, nationwide study. Cancer. 2018;124(9):1964‐1972. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

