Determinants of early neonatal outcomes after emergency cesarean delivery at Hawassa University comprehensive specialised hospital, Hawassa, Ethiopia
- PMID: 35324921
- PMCID: PMC8947390
- DOI: 10.1371/journal.pone.0263837
Determinants of early neonatal outcomes after emergency cesarean delivery at Hawassa University comprehensive specialised hospital, Hawassa, Ethiopia
Abstract
Background: Neonatal mortality after cesarean delivery is three folds higher than mortality after vaginal births. Post cesarean early neonatal outcomes are associated with preoperative and intraoperative fetomaternal factors which are preventable in the majority of cases.
Objective: To identify determinants of early neonatal outcomes after emergency cesarean delivery at Hawassa University Comprehensive Specialized Hospital, Hawassa, Southern Ethiopia.
Method: Institution based cross sectional study was conducted on 270 emergency cesarean deliveries. Data were collected by using a pretested questionnaire by trained data collectors. Descriptive analysis was used to see the nature of the characteristics of interests. Pearson chi-square-test was used to check presence of association between independent and outcome variables. Bivariate analysis was used to sort out variables at p values less than 0.05 for multivariate logistic regression. Significance level was obtained using odds ratio with 95% CI and p value < 0.05.
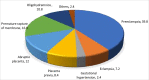
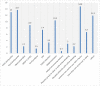
Results: The prevalence of adverse early neonatal outcome after emergency cesarean delivery was 26.7%. Around 11% of newborns had low (<7) fifth minute Apgar score and more than one-third (34.8%) of them admitted to neonatal intensive care unit for more than 24 hours. Fifteen (5.6%) newborns died within their first seven days of life. Neonates with a preoperative meconium-stained amniotic fluid and low birth weight (< 2500 grams) had greater odds of having adverse early neonatal outcome with (AOR = 6.37; 95% CI: 2.64, 15.34) and (AOR = 14.00; 95% CI: 3.64, 53.84) respectively.
Conclusion: The prevalence of adverse early neonatal outcome is high in this study and meconium-stained amniotic fluid during labor as well as low birth weight were the leading predictors of adverse early neonatal outcome during emergency cesarean delivery.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Prevalence and factors associated with low 5th minute APGAR score among mothers who birth through emergency cesarean section: prospective cross-sectional study in Ethiopia.BMC Pregnancy Childbirth. 2025 Mar 25;25(1):342. doi: 10.1186/s12884-025-07456-9. BMC Pregnancy Childbirth. 2025. PMID: 40133944 Free PMC article.
-
Determinants of low fifth minute Apgar score among newborns delivered by cesarean section at Wolaita Sodo University Comprehensive Specialized Hospital, Southern Ethiopia: an unmatched case control study.BMC Pregnancy Childbirth. 2022 Aug 26;22(1):665. doi: 10.1186/s12884-022-04999-z. BMC Pregnancy Childbirth. 2022. PMID: 36028804 Free PMC article.
-
Predictors of neonatal mortality among neonates admitted to the neonatal intensive care unit at Hawassa University Comprehensive Specialized Hospital, Sidama regional state, Ethiopia.BMC Pediatr. 2024 Apr 3;24(1):237. doi: 10.1186/s12887-024-04689-z. BMC Pediatr. 2024. PMID: 38570750 Free PMC article.
-
Neonatal near misses and associated factors among mother's who give a live neonate at Hawassa City governmental hospitals, 2019: a facility based cross-sectional study design.BMC Pregnancy Childbirth. 2021 Feb 12;21(1):125. doi: 10.1186/s12884-021-03601-2. BMC Pregnancy Childbirth. 2021. PMID: 33579215 Free PMC article.
-
Determinants of low Apgar score among newborns delivered by Cesarean section in Nigist Eleni Mohammed memorial specialized hospital, Southern Ethiopia.Sci Rep. 2024 May 30;14(1):12420. doi: 10.1038/s41598-024-62223-8. Sci Rep. 2024. PMID: 38816451 Free PMC article.
Cited by
-
Maternal and neonatal outcomes of dichorionic twin pregnancies achieved with assisted reproductive technology: meta-analysis of contemporary data.J Assist Reprod Genet. 2024 Mar;41(3):581-589. doi: 10.1007/s10815-024-03035-7. Epub 2024 Mar 21. J Assist Reprod Genet. 2024. PMID: 38285318 Free PMC article. Review.
-
Prevalence of emergency caesarean delivery and its predictors among women who give birth in Ethiopia using further analysis of EDHS 2016 data: A mixed effect model.PLoS One. 2024 May 16;19(5):e0300528. doi: 10.1371/journal.pone.0300528. eCollection 2024. PLoS One. 2024. PMID: 38753832 Free PMC article.
-
Determinant of adverse early neonatal outcomes following emergency cesarean section in North West, Ethiopia: institutional-based case-control study.BMC Pregnancy Childbirth. 2024 Dec 30;24(1):881. doi: 10.1186/s12884-024-07037-2. BMC Pregnancy Childbirth. 2024. PMID: 39734223 Free PMC article.
-
Implementation of a crash cesarean section policy and its impact on maternal and neonatal outcomes at King Abdulaziz University Hospital: A retrospective study.Medicine (Baltimore). 2024 Nov 29;103(48):e40645. doi: 10.1097/MD.0000000000040645. Medicine (Baltimore). 2024. PMID: 39612466 Free PMC article.
-
Prevalence and factors associated with low 5th minute APGAR score among mothers who birth through emergency cesarean section: prospective cross-sectional study in Ethiopia.BMC Pregnancy Childbirth. 2025 Mar 25;25(1):342. doi: 10.1186/s12884-025-07456-9. BMC Pregnancy Childbirth. 2025. PMID: 40133944 Free PMC article.
References
-
- Gabbe SG, Niebyl JR, Simpson JL, Landon MB, Galan HL, Jauniaux ER, et al.. Obstetrics: normal and problem pregnancies e-book: Elsevier Health Sciences; 2016.
-
- WHO U, UNICEF. AMDD (2009) Monitoring emergency obstetric care: a handbook. Geneva: WHO. 2009.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical