Peri-Implant Surgical Treatment Downregulates the Expression of sTREM-1 and MMP-8 in Patients with Peri-Implantitis: A Prospective Study
- PMID: 35329310
- PMCID: PMC8955840
- DOI: 10.3390/ijerph19063627
Peri-Implant Surgical Treatment Downregulates the Expression of sTREM-1 and MMP-8 in Patients with Peri-Implantitis: A Prospective Study
Abstract
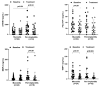
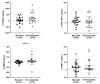
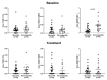
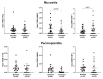
sTREM-1 and its ligand PGLYRP1 play an essential role in the inflammatory process around teeth and implants. In this study, we aimed to evaluate the impact of peri-implant treatment on the salivary levels of the sTREM-1/PGLYRP-1/MMP-8 axis after 3 months. A total of 42 participants (with a mean age of 61 years old ± 7.3) were enrolled in this longitudinal study, 24 having peri-implant mucositis (MU) and 18 having peri-implantitis (PI). Clinical peri-implant parameters, such as probing pocket depth (PPD), % of plaque, and bleeding on probing (BOP), and the whole unstimulated saliva samples were evaluated at baseline and 3 months after treatment. The MU group received nonsurgical peri-implant treatment, while the PI group received open-flap procedures. The levels of sTREM-1, PGLYRP-1, MMP-8, and TIMP-1 were analyzed using enzyme-linked immunosorbent assays. BOP, plaque levels, and PPD significantly reduced after treatment in both groups. A significant decrease in the salivary levels of sTREM-1, MMP-8, and TIMP-1 in the PI group and PGLYRP1 and TIMP-1 in the MU group were observed. Salivary levels of sTREM-1 were significantly reduced in patients with PI but not with MU. Additionally, peri-implant treatment had a significantly higher impact on MMP-8 reduction in patients with PI than in those with MU.
Keywords: MMP-8; PGLYRP-1; peri-implant mucositis; peri-implant treatment; peri-implantitis; sTREM-1.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
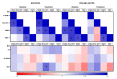
References
-
- Berglundh T., Armitage G., Araujo M.G., Avila-Ortiz G., Blanco J., Camargo P.M., Chen S., Cochran D., Derks J., Figuero E., et al. Peri-implant diseases and conditions: Consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J. Periodontol. 2018;89:S313–S318. doi: 10.1002/JPER.17-0739. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

