Angiogenic Imbalance and Inflammatory Biomarkers in the Prediction of Hypertension as Well as Obstetric and Perinatal Complications in Women with Gestational Diabetes Mellitus
- PMID: 35329840
- PMCID: PMC8953606
- DOI: 10.3390/jcm11061514
Angiogenic Imbalance and Inflammatory Biomarkers in the Prediction of Hypertension as Well as Obstetric and Perinatal Complications in Women with Gestational Diabetes Mellitus
Abstract
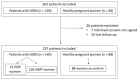
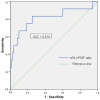
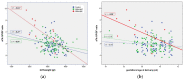
Gestational diabetes mellitus (GDM) increases the risk of hypertensive disorders of pregnancy (HDP). We aimed to analyze the altered inflammatory markers and angiogenic factors among women with GDM to identify pregnant women at higher risk of developing HDP. Methods: This was a prospective study of 149 women without hypertension diagnosed in the third trimester with GDM. Inflammatory markers and angiogenic factors were measured at 28−32 weeks of pregnancy. Obstetric and perinatal outcomes were evaluated. Results: More than eight percent of the women developed HDP. Higher levels of the soluble fms-like tyrosine kinase-1/placental growth factor (sFlt-1/PIGF) ratio (4.9 ± 2.6 versus 2.3 ± 1.3, respectively; p < 0.001) and leptin (10.9 ± 0.8 versus 10.08 ± 1.1, respectively; p = 0.038), as well as lower levels of adiponectin (10.5 ± 1.3 versus 12.9 ± 2.7, respectively; p = 0.031), were seen in women who developed HDP versus normotensive women with GDM. A multivariable logistic regression analysis showed that adiponectin had a protective effect with 0.45-fold odds (0.23−0.83; p = 0.012), and that the sFlt-1/PIGF ratio was associated with 2.70-fold odds of developing HDP (CI 95%: 1.24−5.86; p = 0.012). Conclusion: An increase in angiogenic imbalance in the sFlt-1/PIGF ratio in women with GDM was detected and may be an indicator of developing HDP in addition to any subsequent obstetric and perinatal complications.
Keywords: angiogenic factors; gestational diabetes; hypertensive disorders of pregnancy; sFlt-1/PIGF ratio.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures
References
-
- Regitz-Zagrosek V., Roos-Hesselink J.W., Bauersachs J., Blomström-Lundqvist C., Cífková R., De Bonis M., Iung B., Johnson M.R., Kintscher U., Kranke P., et al. 2018 ESC Guidelines for the Management of Cardiovascular Diseases during Pregnancy. Eur. Heart J. 2018;39:3165–3241. doi: 10.1093/eurheartj/ehy340. - DOI - PubMed
-
- Kelly C.B., Hookham M.B., Yu J.Y., Lockhart S.M., Du M., Jenkins A., Nankervis A., Hanssen K.F., Henriksen T., Garg S.K., et al. Circulating Adipokines Are Associated with Pre-Eclampsia in Women with Type 1 Diabetes. Diabetologia. 2017;60:2514–2524. doi: 10.1007/s00125-017-4415-z. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

