The Survival of Septic Patients with Compensated Liver Cirrhosis Is Not Inferior to That of Septic Patients without Liver Cirrhosis: A Propensity Score Matching Analysis
- PMID: 35329955
- PMCID: PMC8951259
- DOI: 10.3390/jcm11061629
The Survival of Septic Patients with Compensated Liver Cirrhosis Is Not Inferior to That of Septic Patients without Liver Cirrhosis: A Propensity Score Matching Analysis
Abstract
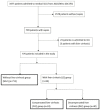
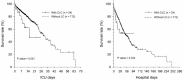
Background: We aimed to determine whether septic patients with liver cirrhosis (LC) had worse survival than septic patients without liver cirrhosis (WLC). We also investigated the survival of septic patients with compensated liver cirrhosis (CLC) and decompensated liver cirrhosis (DLC). Methods: This study enrolled 776 consecutive adult patients with sepsis admitted to the medical intensive care units of a tertiary referral hospital. Clinical factors and laboratory data were collected for analysis. Propensity scoring was also used for the control of selection bias. The variables included in the propensity model were age, sex, presence of diabetes mellitus, hypertension, cardiovascular accident, chronic kidney disease, malignancy, APCHE II (Acute Physiology and Chronic Health Evaluation) score, hemoglobin, and platelet data on the day when sepsis was confirmed. Seven-day, ICU, and hospital mortality were analyzed after correcting for these confounding factors. Results: Of the 776 septic patients, 64 (8.2%) septic patients presented with LC. Patients were divided into two groups—LC (n = 64) and WLC (n = 712)—which presented different rates of hospital mortality (LC: 62.5% vs. WLC: 41.0%, p = 0.001). We further separated septic patients with LC into two groups: patients with CLC (n = 24) and those with DLC (n = 40). After propensity score matching, the survival of septic patients with CLC (63.6%) was not inferior to patients WLC (54.5%) (p = 0.411). Patients with DLC had more hospital mortality, even after matching (p < 0.05). The Quick SOFA (qSOFA) score, SOFA score, and sub-SOFA score were also comparable between groups. SOFA scores were not significantly different between the CLC and WLC groups after matching. Poor SOFA scores were observed in the DLC group on days 3 and 7 after matching (p < 0.05). Conclusions: Septic patients with LC had higher mortality compared to patients WLC before matching. However, after propensity score matching, the survival of septic patients with CLC was non-inferior to patients WLC.
Keywords: intensive care; liver cirrhosis; propensity score; sepsis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

Similar articles
-
[Predictive value of four different scoring systems for septic patient's outcome: a retrospective analysis with 311 patients].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2017 Feb;29(2):133-138. doi: 10.3760/cma.j.issn.2095-4352.2017.02.008. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2017. PMID: 28625260 Chinese.
-
Assessment of Sepsis-3 criteria and quick SOFA in patients with cirrhosis and bacterial infections.Gut. 2018 Oct;67(10):1892-1899. doi: 10.1136/gutjnl-2017-314324. Epub 2017 Aug 31. Gut. 2018. PMID: 28860348
-
[Combined prognostic value of serum lactic acid, procalcitonin and severity score for short-term prognosis of septic shock patients].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2021 Mar;33(3):281-285. doi: 10.3760/cma.j.cn121430-20201113-00715. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2021. PMID: 33834968 Chinese.
-
Increased Survival for Patients With Cirrhosis and Organ Failure in Liver Intensive Care and Validation of the Chronic Liver Failure-Sequential Organ Failure Scoring System.Clin Gastroenterol Hepatol. 2015 Jul;13(7):1353-1360.e8. doi: 10.1016/j.cgh.2014.08.041. Epub 2014 Sep 21. Clin Gastroenterol Hepatol. 2015. PMID: 25240417
-
[Lactic acid, lactate clearance and procalcitonin in assessing the severity and predicting prognosis in sepsis].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2020 Apr;32(4):449-453. doi: 10.3760/cma.j.cn121430-20200129-00086. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2020. PMID: 32527351 Chinese.
Cited by
-
Association of Hypernatremia with Immune Profiles and Clinical Outcomes in Adult Intensive Care Unit Patients with Sepsis.Biomedicines. 2022 Sep 14;10(9):2285. doi: 10.3390/biomedicines10092285. Biomedicines. 2022. PMID: 36140385 Free PMC article.
-
Management of sepsis in a cirrhotic patient admitted to the intensive care unit: A systematic literature review.World J Hepatol. 2023 Jun 27;15(6):850-866. doi: 10.4254/wjh.v15.i6.850. World J Hepatol. 2023. PMID: 37397933 Free PMC article.
References
-
- Fang W.F., Douglas I.S., Chen Y.M., Lin C.Y., Kao H.C., Fang Y.T., Huang C.H., Chang Y.T., Huang K.T., Wang Y.H., et al. Development and validation of immune dysfunction score to predict 28-day mortality of sepsis patients. PLoS ONE. 2017;12:e0187088. doi: 10.1371/journal.pone.0187088. - DOI - PMC - PubMed
-
- Fang W.F., Chen Y.M., Lin C.Y., Huang K.T., Kao H.C., Fang Y.T., Huang C.H., Chang Y.T., Wang Y.H., Wang C.C., et al. Immune profiles and clinical outcomes between sepsis patients with or without active cancer requiring admission to intensive care units. PLoS ONE. 2017;12:e0179749. doi: 10.1371/journal.pone.0179749. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

