COVID-19 Patients Presenting with Post-Intubation Upper Airway Complications: A Parallel Epidemic?
- PMID: 35330044
- PMCID: PMC8948992
- DOI: 10.3390/jcm11061719
COVID-19 Patients Presenting with Post-Intubation Upper Airway Complications: A Parallel Epidemic?
Abstract
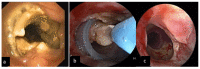
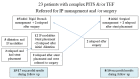
During the current pandemic, we witnessed a rise of post-intubation tracheal stenosis (PITS) in patients intubated due to COVID-19. We prospectively analyzed data from patients referred to our institution during the last 18 months for severe symptomatic post-intubation upper airway complications. Interdisciplinary bronchoscopic and/or surgical management was offered. Twenty-three patients with PITS and/or tracheoesophageal fistulae were included. They had undergone 31.85 (±22.7) days of ICU hospitalization and 17.35 (±7.4) days of intubation. Tracheal stenoses were mostly complex, located in the subglottic or mid-tracheal area. A total of 83% of patients had fracture and distortion of the tracheal wall. Fifteen patients were initially treated with rigid bronchoscopic modalities and/or stent placement and eight patients with tracheal resection-anastomosis. Post-treatment relapse in two of the bronchoscopically treated patients required surgery, while two of the surgically treated patients required rigid bronchoscopy and stent placement. Transient, non-life-threatening post-treatment complications developed in 60% of patients and were all managed successfully. The histopathology of the resected tracheal specimens didn't reveal specific alterations in comparison to pre-COVID-era PITS cases. Prolonged intubation, pronation maneuvers, oversized tubes or cuffs, and patient- or disease-specific factors may be pathogenically implicated. An increase of post-COVID PITS is anticipated. Careful prevention, early detection and effective management of these iatrogenic complications are warranted.
Keywords: COVID-19; airway complications; intubation; tracheal stenosis; tracheoesophageal fistula; tracheostomy.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



References
-
- Kowalski L.P., Sanabria A., Ridge J.A., Ng W.T., Bree R., Rinaldo A., Takes R.P., Mäkitie A.A., Carvalho A.L., Bradford C.R., et al. COVID-19 pandemic: Effects and evidence-based recommendations for otolaryngology and head and neck surgery practice. Head Neck. 2020;42:1259–1267. doi: 10.1002/hed.26164. - DOI - PMC - PubMed
-
- Sommer D.D., Engels P.T., Weitzel E., Khalili S., Corsten M., Tewfik M.A., Fung K., Cote D., Gupta M., Sne N., et al. Recommendations from the CSO-HNS taskforce on performance of tracheotomy during the COVID-19 pandemic. J. Otolaryngol. Head Neck Surg. 2020;49:23. doi: 10.1186/s40463-020-00414-9. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

