Radiogenomic Predictors of Recurrence in Glioblastoma-A Systematic Review
- PMID: 35330402
- PMCID: PMC8952807
- DOI: 10.3390/jpm12030402
Radiogenomic Predictors of Recurrence in Glioblastoma-A Systematic Review
Abstract
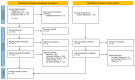
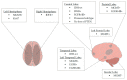
Glioblastoma, as the most aggressive brain tumor, is associated with a poor prognosis and outcome. To optimize prognosis and clinical therapy decisions, there is an urgent need to stratify patients with increased risk for recurrent tumors and low therapeutic success to optimize individual treatment. Radiogenomics establishes a link between radiological and pathological information. This review provides a state-of-the-art picture illustrating the latest developments in the use of radiogenomic markers regarding prognosis and their potential for monitoring recurrence. Databases PubMed, Google Scholar, and Cochrane Library were searched. Inclusion criteria were defined as diagnosis of glioblastoma with histopathological and radiological follow-up. Out of 321 reviewed articles, 43 articles met these inclusion criteria. Included studies were analyzed for the frequency of radiological and molecular tumor markers whereby radiogenomic associations were analyzed. Six main associations were described: radiogenomic prognosis, MGMT status, IDH, EGFR status, molecular subgroups, and tumor location. Prospective studies analyzing prognostic features of glioblastoma together with radiological features are lacking. By reviewing the progress in the development of radiogenomic markers, we provide insights into the potential efficacy of such an approach for clinical routine use eventually enabling early identification of glioblastoma recurrence and therefore supporting a further personalized monitoring and treatment strategy.
Keywords: GBM; glioblastoma; gliomas; imaging genomics; magnetic resonance imaging; molecular markers; neuro-oncology; radiogenomics; radiology; radiomics; recurrence.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures
References
-
- Wen P.Y., Weller M., Lee E.Q., Alexander B.M., Barnholtz-Sloan J.S., Barthel F.P., Batchelor T.T., Bindra R.S., Chang S.M., Chiocca E.A., et al. Glioblastoma in adults: A Society for Neuro-Oncology (SNO) and European Society of Neuro-Oncology (EANO) consensus review on current management and future directions. Neuro-Oncology. 2020;22:1073–1113. doi: 10.1093/neuonc/noaa106. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

