Methods of Assessing Frailty in the Critically Ill: A Systematic Review of the Current Literature
- PMID: 35339999
- PMCID: PMC9808663
- DOI: 10.1159/000523674
Methods of Assessing Frailty in the Critically Ill: A Systematic Review of the Current Literature
Abstract
Introduction: As new treatments have become established, more frail pre-ICU patients are being admitted to intensive care units (ICUs); this is creating new challenges to provide adequate care and to ensure that resources are allocated in an ethical and economical manner. This systematic review evaluates the current standard for assessing frailty on the ICU, including methods of assessment, time point of measurements, and cut-offs.
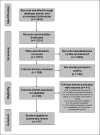
Methods: A systematic search was conducted on MEDLINE, Clinical Trials, Cochrane Library, and Embase. Randomized and non-randomized controlled studies were included that evaluated diagnostic tools and ICU outcomes for frailty. Exclusion criteria were the following: studies without baseline assessment of frailty on ICU admission, studies in paediatric patients or pregnant women, and studies that targeted very narrow populations of ICU patients. Eligible articles were included until January 31, 2021. Methodological quality was assessed using the Newcastle-Ottawa Scale. No meta-analysis was performed, due to heterogeneity.
Results: N = 57 articles (253,376 patients) were included using 19 different methods to assess frailty or a surrogate. Frailty on ICU admission was most frequently detected using the Clinical Frailty Scale (CFS) (n = 35, 60.3%), the Frailty Index (n = 5, 8.6%), and Fried's frailty phenotype (n = 6, 10.3%). N = 22 (37.9%) studies assessed functional status. Cut-offs, time points, and manner of baseline assessment of frailty on ICU admission varied widely. Frailty on ICU admission was associated with short- and long-term mortality, functional and cognitive impairment, increased health care dependency, and impaired quality of life post-ICU discharge.
Conclusions: Frailty assessment on the ICU is heterogeneous with respect to methods, cut-offs, and time points. The CFS may best reflect frailty in the ICU. Frailty assessments should be harmonized and performed routinely in the critically ill.
Keywords: Assessment; Critical care; Decision-making; Frailty; Geriatric medicine; Outcome.
© 2022 The Author(s). Published by S. Karger AG, Basel.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Similar articles
-
Sarcopenia and frailty in critical illness.Curr Opin Clin Nutr Metab Care. 2025 May 1;28(3):192-199. doi: 10.1097/MCO.0000000000001123. Epub 2025 Mar 12. Curr Opin Clin Nutr Metab Care. 2025. PMID: 40072495 Free PMC article. Review.
-
Assessing the Usefulness and Validity of Frailty Markers in Critically Ill Adults.Ann Am Thorac Soc. 2017 Jun;14(6):952-959. doi: 10.1513/AnnalsATS.201607-538OC. Ann Am Thorac Soc. 2017. PMID: 28358584 Free PMC article.
-
Clinical Frailty Scale (CFS) reliably stratifies octogenarians in German ICUs: a multicentre prospective cohort study.BMC Geriatr. 2018 Jul 13;18(1):162. doi: 10.1186/s12877-018-0847-7. BMC Geriatr. 2018. PMID: 30005622 Free PMC article.
-
The contribution of frailty, cognition, activity of daily life and comorbidities on outcome in acutely admitted patients over 80 years in European ICUs: the VIP2 study.Intensive Care Med. 2020 Jan;46(1):57-69. doi: 10.1007/s00134-019-05853-1. Epub 2019 Nov 29. Intensive Care Med. 2020. PMID: 31784798 Free PMC article.
-
Association between frailty and clinical outcomes in surgical patients admitted to intensive care units: a systematic review and meta-analysis.Br J Anaesth. 2022 Feb;128(2):258-271. doi: 10.1016/j.bja.2021.11.018. Epub 2021 Dec 17. Br J Anaesth. 2022. PMID: 34924178
Cited by
-
Sarcopenia and frailty in critical illness.Curr Opin Clin Nutr Metab Care. 2025 May 1;28(3):192-199. doi: 10.1097/MCO.0000000000001123. Epub 2025 Mar 12. Curr Opin Clin Nutr Metab Care. 2025. PMID: 40072495 Free PMC article. Review.
-
Clinical frailty scale at ICU discharge predicts ICU readmission and post-ICU mortality: A retrospective single-center study.Medicine (Baltimore). 2025 Jun 20;104(25):e42955. doi: 10.1097/MD.0000000000042955. Medicine (Baltimore). 2025. PMID: 40550056 Free PMC article.
-
Frailty, Outcomes, Recovery and Care Steps of Critically Ill Patients (FORECAST): a prospective, multi-centre, cohort study.Intensive Care Med. 2024 Jul;50(7):1064-1074. doi: 10.1007/s00134-024-07404-9. Epub 2024 May 15. Intensive Care Med. 2024. PMID: 38748266 Free PMC article.
-
Association between frailty index based on laboratory tests and all-cause mortality in critically ill patients with heart failure.ESC Heart Fail. 2024 Dec;11(6):3662-3673. doi: 10.1002/ehf2.14948. Epub 2024 Jul 9. ESC Heart Fail. 2024. PMID: 38979803 Free PMC article.
-
Age- and sex-specific associations of frailty with mortality and healthcare utilization in community-dwelling adults from ontario, Canada.BMC Geriatr. 2024 Mar 4;24(1):223. doi: 10.1186/s12877-024-04842-4. BMC Geriatr. 2024. PMID: 38438981 Free PMC article.
References
-
- Ihra GC, Lehberger J, Hochrieser H, Bauer P, Schmutz R, Metnitz B, et al. Development of demographics and outcome of very old critically ill patients admitted to intensive care units. Intensive Care Med. 2012 Apr;38((4)):620–626. - PubMed
-
- Andersen FH, Flaatten H, Klepstad P, Follestad T, Strand K, Kruger AJ, et al. Long-term outcomes after ICU admission triage in octogenarians. Crit Care Med. 2017 Apr;45((4)):e363–71. - PubMed
-
- Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001 Mar;56((3)):M146–56. - PubMed
-
- Haas LEM, Boumendil A, Flaatten H, Guidet B, Ibarz M, Jung C, et al. Frailty is associated with long-term outcome in patients with sepsis who are over 80 years old: results from an observational study in 241 European ICUs. Age Ageing. 2021;50((5)):1719–1727. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials