Neurodevelopment in Children Exposed to Zika in utero: Clinical and Molecular Aspects
- PMID: 35350244
- PMCID: PMC8957982
- DOI: 10.3389/fgene.2022.758715
Neurodevelopment in Children Exposed to Zika in utero: Clinical and Molecular Aspects
Abstract
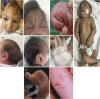
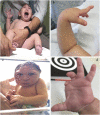
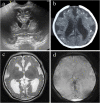
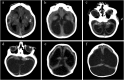
Five years after the identification of Zika virus as a human teratogen, we reviewed the early clinical manifestations, collectively called congenital Zika syndrome (CZS). Children with CZS have a very poor prognosis with extremely low performance in motor, cognitive, and language development domains, and practically all feature severe forms of cerebral palsy. However, these manifestations are the tip of the iceberg, with some children presenting milder forms of deficits. Additionally, neurodevelopment can be in the normal range in the majority of the non-microcephalic children born without brain or eye abnormalities. Vertical transmission and the resulting disruption in development of the brain are much less frequent when maternal infection occurs in the second half of the pregnancy. Experimental studies have alerted to the possibility of other behavioral outcomes both in prenatally infected children and in postnatal and adult infections. Cofactors play a vital role in the development of CZS and involve genetic, environmental, nutritional, and social determinants leading to the asymmetric distribution of cases. Some of these social variables also limit access to multidisciplinary professional treatment.
Keywords: cerebral palsy; epilepsy; eye; microcephaly; neurodevelopement; zika (ZIKV).
Copyright © 2022 Schuler-Faccini, del Campo, García-Alix, Ventura, Boquett, van der Linden, Pessoa, van der Linden Júnior, Ventura, Leal, Kowalski, Rodrigues Gerzson, Skilhan de Almeida, Santi, Beys-da-Silva, Quincozes-Santos, Guimarães, Garcez, Gomes, Vianna, Anjos da Silva, Fraga, Vieira Sanseverino, Muotri, Lopes da Rosa, Abeche, Marcolongo-Pereira and Souza.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
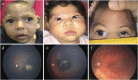

References
-
- Abtibol-Bernardino M. R., de Almeida Peixoto L. d. F. A., de Oliveira G. A., de Almeida T. F., Rodrigues G. R. I., Otani R. H., et al. (2020). Neurological Findings in Children without Congenital Microcephaly Exposed to Zika Virus In Utero: A Case Series Study. Viruses 12 (11), 1335. 10.3390/v12111335 - DOI - PMC - PubMed
-
- Adebanjo T., Godfred-Cato S., Viens L., Fischer M., Staples J. E., Kuhnert-Tallman W., et al. (2017). Update: Interim Guidance for the Diagnosis, Evaluation, and Management of Infants with Possible Congenital Zika Virus Infection - United States, October 2017. MMWR Morb Mortal Wkly Rep. 66 (41), 1089–1099. 10.15585/mmwr.mm6641a1 - DOI - PMC - PubMed
-
- Ades A. E., Brickley E. B., Alexander N., Brown D., Jaenisch T., Miranda-Filho D. d. B., et al. (2020). Zika Virus Infection in Pregnancy: a Protocol for the Joint Analysis of the Prospective Cohort Studies of the ZIKAlliance, ZikaPLAN and ZIKAction Consortia. BMJ open 10 (12), e035307. 10.1136/bmjopen-2019-035307 - DOI - PMC - PubMed

