Cancer risks among studies of medical diagnostic radiation exposure in early life without quantitative estimates of dose
- PMID: 35351505
- PMCID: PMC9167801
- DOI: 10.1016/j.scitotenv.2022.154723
Cancer risks among studies of medical diagnostic radiation exposure in early life without quantitative estimates of dose
Abstract
Background: There is accumulating evidence of excess risk of cancer in various populations exposed at acute doses below several tens of mSv or doses received over a protracted period. There is also evidence that relative risks are generally higher after radiation exposures in utero or in childhood.
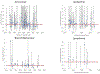
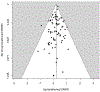
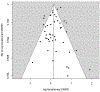
Methods and findings: We reviewed and summarised evidence from 89 studies of cancer following medical diagnostic exposure in utero or in childhood, in which no direct estimates of radiation dose are available. In all of the populations studied exposure was to sparsely ionizing radiation (X-rays). Several of the early studies of in utero exposure exhibit modest but statistically significant excess risks of several types of childhood cancer. There is a highly significant (p < 0.0005) negative trend of odds ratio with calendar period of study, so that more recent studies tend to exhibit reduced excess risk. There is no significant inter-study heterogeneity (p > 0.3). In relation to postnatal exposure there are significant excess risks of leukaemia, brain and solid cancers, with indications of variations in risk by cancer type (p = 0.07) and type of exposure (p = 0.02), with fluoroscopy and computed tomography scans associated with the highest excess risk. However, there is highly significant inter-study heterogeneity (p < 0.01) for all cancer endpoints and all but one type of exposure, although no significant risk trend with calendar period of study.
Conclusions: Overall, this large body of data relating to medical diagnostic radiation exposure in utero provides support for an associated excess risk of childhood cancer. However, the pronounced heterogeneity in studies of postnatal diagnostic exposure, the implied uncertainty as to the meaning of summary measures, and the distinct possibilities of bias, substantially reduce the strength of the evidence from the associations we observe between radiation imaging in childhood and the subsequent risk of cancer being causally related to radiation exposure.
Keywords: Childhood; In utero; Radiation; cancer risk.
Crown Copyright © 2022. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Declaration of competing interest The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: Richard Wakeford receives a consultancy fee as a member of the Technical Working Party of the Compensation Scheme for Radiation-linked Diseases (http://www.csrld.org.uk). No other authors report conflicts of interest.
Figures
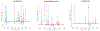
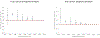
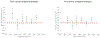
Similar articles
-
Review of the risk of cancer following low and moderate doses of sparsely ionising radiation received in early life in groups with individually estimated doses.Environ Int. 2022 Jan 15;159:106983. doi: 10.1016/j.envint.2021.106983. Epub 2021 Dec 24. Environ Int. 2022. PMID: 34959181 Free PMC article. Review.
-
Early life ionizing radiation exposure and cancer risks: systematic review and meta-analysis.Pediatr Radiol. 2021 Jan;51(1):45-56. doi: 10.1007/s00247-020-04803-0. Epub 2020 Sep 10. Pediatr Radiol. 2021. PMID: 32910229
-
Epidemiological Studies of Low-Dose Ionizing Radiation and Cancer: Summary Bias Assessment and Meta-Analysis.J Natl Cancer Inst Monogr. 2020 Jul 1;2020(56):188-200. doi: 10.1093/jncimonographs/lgaa010. J Natl Cancer Inst Monogr. 2020. PMID: 32657347 Free PMC article.
-
Leukaemia and myeloid malignancy among people exposed to low doses (<100 mSv) of ionising radiation during childhood: a pooled analysis of nine historical cohort studies.Lancet Haematol. 2018 Aug;5(8):e346-e358. doi: 10.1016/S2352-3026(18)30092-9. Epub 2018 Jul 17. Lancet Haematol. 2018. PMID: 30026010 Free PMC article.
-
Radiation exposure from CT scans in childhood and subsequent risk of leukaemia and brain tumours: a retrospective cohort study.Lancet. 2012 Aug 4;380(9840):499-505. doi: 10.1016/S0140-6736(12)60815-0. Epub 2012 Jun 7. Lancet. 2012. PMID: 22681860 Free PMC article.
Cited by
-
A generalisation of the method of regression calibration and comparison with Bayesian and frequentist model averaging methods.ArXiv [Preprint]. 2024 Mar 13:arXiv:2312.02215v3. ArXiv. 2024. Update in: Sci Rep. 2024 Mar 19;14(1):6613. doi: 10.1038/s41598-024-56967-6. PMID: 38196750 Free PMC article. Updated. Preprint.
-
Low-dose radiotherapy for COVID-19 pneumonia and cancer: summary of a recent symposium and future perspectives.Int J Radiat Biol. 2023;99(2):357-371. doi: 10.1080/09553002.2022.2074165. Epub 2022 May 26. Int J Radiat Biol. 2023. PMID: 35511152 Free PMC article.
-
The Evidence for Excess Risk of Cancer and Non-Cancer Disease at Low Doses and Dose Rates.Radiat Res. 2022 Dec 1;198(6):615-624. doi: 10.1667/RADE-22-00132.1. Radiat Res. 2022. PMID: 36136740 Free PMC article.
-
A generalisation of the method of regression calibration.Res Sq [Preprint]. 2023 Aug 18:rs.3.rs-3248694. doi: 10.21203/rs.3.rs-3248694/v1. Res Sq. 2023. Update in: Sci Rep. 2023 Sep 13;13(1):15127. doi: 10.1038/s41598-023-42283-y. PMID: 37645976 Free PMC article. Updated. Preprint.
-
Radiotherapy for non-cancer diseases: benefits and long-term risks.Int J Radiat Biol. 2024;100(4):505-526. doi: 10.1080/09553002.2023.2295966. Epub 2024 Jan 5. Int J Radiat Biol. 2024. PMID: 38180039 Free PMC article. Review.
References
-
- Abalo KD, Rage E, Leuraud K, Richardson DB, Le Pointe HD, Laurier D, et al. Early life ionizing radiation exposure and cancer risks: systematic review and meta-analysis. Pediatr Radiol 2021; 51: 45–56. - PubMed
-
- Ager EA, Schuman LM, Wallace HM, Rosenfield AB, Gullen WH. An epidemiological study of childhood leukemia. J. Chronic Dis 1965; 18: 113–32. - PubMed
-
- Armstrong B, Brenner DJ, Baverstock K, Cardis E, Green A, Guilmette RA, et al. Radiation. Volume 100D. A review of human carcinogens. Lyon, France: International Agency for Research on Cancer, 2012.
-
- Baaken D, Hammer GP, Seidenbusch MC, Schneider K, Spix C, Blettner M, et al. Second follow-up of a German cohort on childhood cancer incidence after exposure to postnatal diagnostic x-ray. J Radiol Prot 2019; 39: 1074–1091. - PubMed
-
- Bailey HD, Armstrong BK, De Klerk NH, Fritschi L, Attia J, Lockwood L, et al. Exposure to diagnostic radiological procedures and the risk of childhood acute lymphoblastic leukemia. Cancer Epidemiology Biomarkers and Prevention 2010; 19: 2897–2909. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

