Wearable Photoplethysmography for Cardiovascular Monitoring
- PMID: 35356509
- PMCID: PMC7612541
- DOI: 10.1109/JPROC.2022.3149785
Wearable Photoplethysmography for Cardiovascular Monitoring
Abstract
Smart wearables provide an opportunity to monitor health in daily life and are emerging as potential tools for detecting cardiovascular disease (CVD). Wearables such as fitness bands and smartwatches routinely monitor the photoplethysmogram signal, an optical measure of the arterial pulse wave that is strongly influenced by the heart and blood vessels. In this survey, we summarize the fundamentals of wearable photoplethysmography and its analysis, identify its potential clinical applications, and outline pressing directions for future research in order to realize its full potential for tackling CVD.
Keywords: Cardiovascular (CV); photoplethysmogram (PPG); pulse wave; sensor; signal processing; smartwatch.
Figures

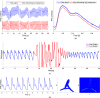
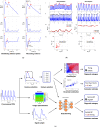
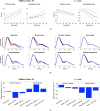
References
-
- Cisco. (2019). Cisco Visual Networking Index (VNI) Global Mobile Data Traffic Forecast Update, 2017–2022 White Paper. Accessed: Mar. 15, 2021. [Online]. Available: https://s3.amazonaws.com/media.mediapost.com/uploads/CiscoForecast.pdf
-
- Gartner. (2021). Gartner Forecasts Global Spending on Wearable Devices to Total $81.5 Billion in 2021. Accessed: Mar. 15, 2021. [Online]. Available: https://www.gartner.com/en/newsroom/press-releases/2021-01-11-gartner-fo...
Grants and funding
LinkOut - more resources
Full Text Sources
