Brief behavioral treatment for insomnia decreases trauma-related nightmare frequency in veterans
- PMID: 35393934
- PMCID: PMC9243281
- DOI: 10.5664/jcsm.10002
Brief behavioral treatment for insomnia decreases trauma-related nightmare frequency in veterans
Abstract
Study objectives: Trauma-related nightmares are highly prevalent among veterans and are associated with higher-severity insomnia and posttraumatic stress disorder. Cognitive behavioral therapy for insomnia (typically 6-8 sessions) has been shown to reduce trauma-related nightmares. Brief behavioral treatment for insomnia (BBTI, 4 sessions) has been found to be comparable to CBT-I in decreasing insomnia severity; however, the effects of BBTI on nightmares have not been investigated. The current study tested the effects of BBTI on both trauma-related nightmares and nontrauma-related bad dreams using an active control group treated using progressive muscle relaxation therapy. In addition, we tested whether baseline trauma-related nightmare frequency and baseline nontrauma-related bad dream frequency moderated changes in insomnia severity.
Methods: Participants were 91 military veterans with insomnia disorder randomized to BBTI or progressive muscle relaxation therapy. Participants reported insomnia severity on the Insomnia Severity Index and reported trauma-related nightmare frequency and nontrauma-related bad dream frequency on the Pittsburgh Sleep Quality Index-PTSD Addendum.
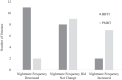
Results: We found that BBTI significantly reduced trauma-related nightmares from baseline to posttreatment, whereas progressive muscle relaxation therapy did not. However, reductions in trauma-related nightmares were not maintained at the 6-month follow up. Neither BBTI nor progressive muscle relaxation therapy reduced nontrauma-related bad dreams from baseline to posttreatment. We also found that neither baseline trauma-related nightmare frequency nor baseline nontrauma-related bad dream frequency moderated changes in insomnia symptom severity.
Conclusions: Findings from the current study suggest that BBTI may help reduce trauma-related nightmares. Further research is needed to better understand the potential mechanisms underlying how improved sleep may reduce trauma-related nightmares.
Clinical trial registration: Registry: ClinicalTrials.gov; Name: Brief Behavioral Insomnia Treatment Study (BBTI); URL: https://clinicaltrials.gov/ct2/show/NCT02571452; Identifier: NCT02571452.
Citation: Ranney RM, Gloria R, Metzler TJ, Huggins J, Neylan TC, Maguen S. Brief behavioral treatment for insomnia decreases trauma-related nightmare frequency in veterans. J Clin Sleep Med. 2022:18(7):1831-1839.
Keywords: Veterans Health Administration; behavioral therapy; insomnia; nightmares; trauma.
© 2022 American Academy of Sleep Medicine.
Conflict of interest statement
All authors have seen and approved this manuscript. Rachel M. Ranney, VA Advanced Postdoctoral Fellow in Mental Illness Research and Treatment, Sierra Pacific (VISN 21) Mental Illness Research Education and Clinical Center, VA San Francisco Health Care System, and the Department of Psychiatry and Behavioral Sciences, University of California, San Francisco School of Medicine. This study was funded by VA Rehabilitation Research and Development grant I01 RX001539 (principal investigator: Maguen). This research is also supported by the Department of Veterans Affairs Office of Academic Affiliations Advanced Fellowship Program in Mental Illness Research and Treatment, the Medical Research Service of the Veterans Affairs San Francisco Health Care System, and the Department of Veterans Affairs Sierra Pacific Mental Illness Research, Education, and Clinical Center. The authors report no conflicts of interest.
Figures
References
-
- Belenky G , Wesensten NJ , Thorne DR , et al . Patterns of performance degradation and restoration during sleep restriction and subsequent recovery: a sleep dose-response study . J Sleep Res. 2003. ; 12 ( 1 ): 1 – 12 . - PubMed
-
- Morphy H , Dunn KM , Lewis M , Boardman HF , Croft PR . Epidemiology of insomnia: a longitudinal study in a UK population . Sleep. 2007. ; 30 ( 3 ): 274 – 280 . - PubMed
-
- Hoge CW , McGurk D , Thomas JL , Cox AL , Engel CC , Castro CA . Mild traumatic brain injury in U.S. soldiers returning from Iraq . N Engl J Med. 2008. ; 358 ( 5 ): 453 – 463 . - PubMed