Improving Access to HLA-Matched Kidney Transplants for African American Patients
- PMID: 35401566
- PMCID: PMC8989073
- DOI: 10.3389/fimmu.2022.832488
Improving Access to HLA-Matched Kidney Transplants for African American Patients
Abstract
Introduction: Kidney transplants fail more often in Black than in non-Black (White, non-Black Hispanic, and Asian) recipients. We used the estimated physicochemical immunogenicity for polymorphic amino acids of donor/recipient HLAs to select weakly immunogenic kidney transplants for Black vs. White or non-Black patients.
Methods: OPTN data for 65,040 donor/recipient pairs over a 20-year period were used to calculate the individual physicochemical immunogenicity by hydrophobic, electrostatic and amino acid mismatch scores (HMS, EMS, AMS) and graft-survival outcomes for Black vs. White or vs. non-Black recipients, using Kaplan-Meier survival and Cox regression analyses. Simulations for re-matching recipients with donors were based on race-adjusted HMS thresholds with clinically achievable allocations.
Results: The retrospective median kidney graft survival was 12.0 years in Black vs. 18.6 years in White (6.6-year difference; p>0.001) and 18.4 years in non-Black (6.4-year difference; p>0.01) recipients. Only 0.7% of Blacks received transplants matched at HLA-A/B/DR/DQ (HMS=0) vs. 8.1% in Whites (p<0.001). Among fully matched Blacks (HMS=0), graft survival was 16.1-years and in well-matched Blacks (HMS ≤ 3.0) it was 14.0-years. Whites had 21.6-years survival at HMS ≤ 3.0 and 18.7-years at HMS ≤ 7.0 whereas non-Blacks had 22.0-year at HMS ≤ 3.0 and 18.7-year at HMS ≤ 7.0, confirming that higher HMS thresholds produced excellent survival. Simulation of ABO-compatible donor-recipient pairs using race-adjusted HMS thresholds identified weakly immunogenic matches at HMS=0 for 6.1% Blacks and 18.0% at HMS ≤ 3.0. Despite prioritizing Black patients, non-Black patients could be matched at the same level as in current allocation (47.0% vs 56.5%, at HMS ≤ 7.0).
Conclusions: Race-adjusted HMS (EMS, AMS)-based allocation increased the number of weakly immunogenic donors for Black patients, while still providing excellent options for non-Black recipients.
Keywords: allocation; human leukocyte antigen; human leukocyte antigen mismatch; immunogenicity; kidney transplantation; race; transplant survival.
Copyright © 2022 Bekbolsynov, Mierzejewska, Khuder, Ekwenna, Rees, Green and Stepkowski.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


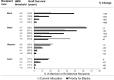
References
-
- Census - Geography Profile: US Census Bureau (2020). Available at: https://data.census.gov/cedsci/profile?q=United%20States&g=0100000US.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

