Platelets, Bacterial Adhesins and the Pneumococcus
- PMID: 35406684
- PMCID: PMC8997422
- DOI: 10.3390/cells11071121
Platelets, Bacterial Adhesins and the Pneumococcus
Abstract
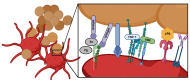
Systemic infections with pathogenic or facultative pathogenic bacteria are associated with activation and aggregation of platelets leading to thrombocytopenia and activation of the clotting system. Bacterial proteins leading to platelet activation and aggregation have been identified, and while platelet receptors are recognized, induced signal transduction cascades are still often unknown. In addition to proteinaceous adhesins, pathogenic bacteria such as Staphylococcus aureus and Streptococcus pneumoniae also produce toxins such as pneumolysin and alpha-hemolysin. They bind to cellular receptors or form pores, which can result in disturbance of physiological functions of platelets. Here, we discuss the bacteria-platelet interplay in the context of adhesin-receptor interactions and platelet-activating bacterial proteins, with a main emphasis on S. aureus and S. pneumoniae. More importantly, we summarize recent findings of how S. aureus toxins and the pore-forming toxin pneumolysin of S. pneumoniae interfere with platelet function. Finally, the relevance of platelet dysfunction due to killing by toxins and potential treatment interventions protecting platelets against cell death are summarized.
Keywords: MSCRAMMs; Staphylococcus aureus; Streptococcus pneumoniae; platelet activation; platelet killing; pneumolysin; pore formation; surface proteins; toxin.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures



References
-
- Robier C. Platelet morphology. J. Lab. Med. 2020;44:231–239. doi: 10.1515/labmed-2020-0007. - DOI
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

