Incidence of Peri-Implantitis and Relationship with Different Conditions: A Retrospective Study
- PMID: 35409826
- PMCID: PMC8998347
- DOI: 10.3390/ijerph19074147
Incidence of Peri-Implantitis and Relationship with Different Conditions: A Retrospective Study
Abstract
Articles on the prevalence of peri-implant diseases showed that 90% of peri-implant tissues had some form of inflammatory response and a prevalence of peri-implantitis from 28% to 51% according to various publications. Objective: To provide an overview of how risk factors can be related with peri-implantitis. Methods: A retrospective longitudinal study including 555 implants placed in 132 patients was evaluated based on the presence of peri-implantitis following the criteria of Renvert et al. 2018. Results: In total, 21 patients (15.9%) suffered peri-implantitis (PPG) and 111 patients (84.1%) did not suffer peri-implantitis (NPG). The results reveal that smokers have a high incidence of peri-implantitis (72.7%) compared to non-smokers (27.3%) (p < 0.0005). Another variable with significant results (p < 0.01) was periodontitis: 50% PPG and 23.9% NPG suffered advanced periodontitis. Systemic diseases such as arterial hypertension, diabetes mellitus, osteoporosis, and cardiovascular diseases do not show a statistically significant influence on the incidence of peri-implantitis. Patients who did not attend their maintenance therapy appointment had an incidence of peri-implantitis of 61.4%, compared to 27.3% in those who attend (p < 0.0001). From the results obtained, we can conclude that relevant factors affect peri-implantitis, such as tobacco habits, moderate and severe periodontitis, and attendance in maintenance therapy.
Keywords: osseointegration; osseous defects; peri-implant disease; peri-implant health; peri-implant mucositis; peri-implantitis; risk factor; risk indicator.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures

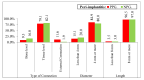
References
-
- Esposito M., Grusovin M.G., Willings M., Coulthard P., Worthington H.V. The effectiveness of immediate, early, and conventional loading of dental implants: A Cochrane systematic review of randomized controlled clinical trials. Int. J. Oral Maxillofac. Implants. 2007;22:893–904. - PubMed
-
- Berglundh T., Persson L., Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J. Clin. Periodontol. 2002;29((Suppl. S3)):197–212. doi: 10.1034/j.1600-051X.29.s3.12.x. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

