Role of Dedicated Subspecialized Radiologists in Multidisciplinary Team Discussions on Lower Gastrointestinal Tract Cancers
- PMID: 35434980
- PMCID: PMC9240296
- DOI: 10.3348/kjr.2021.0680
Role of Dedicated Subspecialized Radiologists in Multidisciplinary Team Discussions on Lower Gastrointestinal Tract Cancers
Abstract
Objective: To determine the impact of dedicated subspecialized radiologists in multidisciplinary team (MDT) discussions on the management of lower gastrointestinal (GI) tract malignancies.
Materials and methods: We retrospectively analyzed the data of 244 patients (mean age ± standard deviation, 61.7 ± 11.9 years) referred to MDT discussions 249 times (i.e., 249 cases, as five patients were discussed twice for different issues) for lower GI tract malignancy including colorectal cancer, small bowel cancer, GI stromal tumor, and GI neuroendocrine tumor between April 2018 and June 2021 in a prospective database. Before the MDT discussions, dedicated GI radiologists reviewed all imaging studies again besides routine clinical reading. The referring clinician's initial diagnosis, initial treatment plan, change in radiologic interpretation compared with the initial radiology report, and the MDT's consensus recommendations for treatment were collected and compared. Factors associated with changes in treatment plans and the implementation of MDT decisions were analyzed.
Results: Of the 249 cases, radiologic interpretation was changed in 73 cases (29.3%) after a review by dedicated GI radiologists, with 78.1% (57/73) resulting in changes in the treatment plan. The treatment plan was changed in 92 cases (36.9%), and the rate of change in the treatment plan was significantly higher in cases with changes in radiologic interpretation than in those without (78.1% [57/73] vs. 19.9% [35/176], p < 0.001). Follow-up records of patients showed that 91.2% (227/249) of MDT recommendations for treatment were implemented. Multiple logistic regression analysis revealed that the nonsurgical approach (vs. surgical approach) decided through MDT discussion was a significant factor for patients being managed differently than the MDT recommendations (Odds ratio, 4.48; p = 0.017).
Conclusion: MDT discussion involving additional review of radiology examinations by dedicated GI radiologists resulted in a change in the treatment plan in 36.9% of cases. Changes in treatment plans were significantly associated with changes in radiologic interpretation.
Keywords: Disease management; Multidisciplinary care team; Neoplasms; Patient care team; Radiologists.
Copyright © 2022 The Korean Society of Radiology.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures

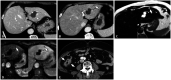
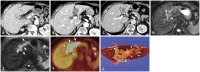
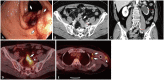
References
-
- Ringborg U, Pierotti M, Storme G, Tursz T European Economic Interest Grouping. Managing cancer in the EU: the Organisation of European Cancer Institutes (OECI) Eur J Cancer. 2008;44:772–773. - PubMed
-
- Wright FC, De Vito C, Langer B, Hunter A Expert Panel on Multidisciplinary Cancer Conference Standards. Multidisciplinary cancer conferences: a systematic review and development of practice standards. Eur J Cancer. 2007;43:1002–1010. - PubMed
-
- Ryan J, Faragher I. Not all patients need to be discussed in a colorectal cancer MDT meeting. Colorectal Dis. 2014;16:520–526. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

