Effects of dietary palmitoleic acid on vascular function in aorta of diabetic mice
- PMID: 35436932
- PMCID: PMC9014575
- DOI: 10.1186/s12902-022-01018-2
Effects of dietary palmitoleic acid on vascular function in aorta of diabetic mice
Abstract
Background: Chronic hyperglycemia in diabetes causes atherosclerosis and progresses to diabetic macroangiopathy, and can lead to coronary heart disease, myocardial infarction and cerebrovascular disease. Palmitoleic acid (POA) is a product of endogenous lipogenesis and is present in fish and vegetable oil. In human and animal studies, POA is reported as a beneficial fatty acid related to insulin sensitivity and glucose tolerance. However, few studies have reported its effects on aortic function in diabetes. Here, we investigated the effects of POA administration on vascular function in KKAy mice, a model of type 2 diabetes.
Methods: Male C57BL/6 J (control) and KKAy (experimental) mice at the age of 14 weeks were used in the present study. For each mouse strain, one group was fed with reference diet and a second group was fed POA-containing diet for 2 weeks. The vascular reactivities of prepared aortic rings were then measured in an organ bath to determine if POA administration changed vascular function in these mice.
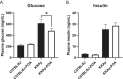
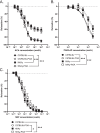
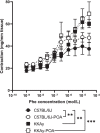
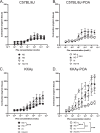
Results: KKAy mice treated with POA exhibited decreased plasma glucose levels compared with mice treated with reference diet. However, endothelium-dependent vasorelaxant responses to acetylcholine and protease-activated receptor 2 activating protein, which are attenuated in the aorta of KKAy mice compared to C57BL/6 J mice under a reference diet, were not affected by a 2-week POA treatment. In addition, assessment of vasoconstriction revealed that the phenylephrine-induced vasoconstrictive response was enhanced in KKAy mice compared to C57BL/6 J mice under a reference diet, but no effect was observed in KKAy mice fed a POA-containing diet. In contrast, there was an increase in vasoconstriction in C57BL/6 J mice fed the POA-containing diet compared to mice fed a reference diet. Furthermore, the vasoconstriction in aorta in both C57BL/6 J and KKAy mice fed a POA-containing diet were further enhanced under hyperglycemic conditions compared to normal glucose conditions in vitro. In the hyperinsulinemic, and hyperinsulinemic combined with hyperglycemic conditions, vasoconstriction was increased in KKAy mice fed with POA.
Conclusion: These results suggest that POA intake enhances vasoconstriction under hyperglycemic and hyperinsulinemic conditions, which are characteristics of type 2 diabetes, and may contribute to increased vascular complications in diabetes.
Keywords: Diabetes; Palmitoleic acid; Thoracic aorta; Vasoconstriction.
© 2022. The Author(s).
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures

Similar articles
-
Eicosapentaenoic acid ethyl ester improves endothelial dysfunction in type 2 diabetic mice.Lipids Health Dis. 2018 May 22;17(1):118. doi: 10.1186/s12944-018-0770-0. Lipids Health Dis. 2018. PMID: 29788974 Free PMC article.
-
Selective inhibition of 11 beta-hydroxysteroid dehydrogenase type 1 improves hepatic insulin sensitivity in hyperglycemic mice strains.Endocrinology. 2003 Nov;144(11):4755-62. doi: 10.1210/en.2003-0344. Epub 2003 Jul 31. Endocrinology. 2003. PMID: 12960099
-
Effect of tempol on altered angiotensin II and acetylcholine-mediated vascular responses in thoracic aorta isolated from rats with insulin resistance.Pharmacol Res. 2006 Mar;53(3):209-15. doi: 10.1016/j.phrs.2005.11.002. Epub 2006 Jan 10. Pharmacol Res. 2006. PMID: 16412660
-
Dietary saury oil reduces hyperglycemia and hyperlipidemia in diabetic KKAy mice and in diet-induced obese C57BL/6J mice by altering gene expression.Lipids. 2011 May;46(5):425-34. doi: 10.1007/s11745-011-3553-1. Epub 2011 Apr 5. Lipids. 2011. PMID: 21465306
-
The Different Insulin-Sensitising and Anti-Inflammatory Effects of Palmitoleic Acid and Oleic Acid in a Prediabetes Model.J Diabetes Res. 2022 Sep 13;2022:4587907. doi: 10.1155/2022/4587907. eCollection 2022. J Diabetes Res. 2022. PMID: 36147256 Free PMC article.
Cited by
-
Low-Molecular-Weight Compounds Produced by the Intestinal Microbiota and Cardiovascular Disease.Int J Mol Sci. 2024 Sep 27;25(19):10397. doi: 10.3390/ijms251910397. Int J Mol Sci. 2024. PMID: 39408727 Free PMC article. Review.
-
Palmitoleic and oleic fatty acids as biomarkers for coronary heart disease: A predictive model.Ir J Med Sci. 2025 Feb;194(1):59-70. doi: 10.1007/s11845-024-03839-7. Epub 2024 Nov 8. Ir J Med Sci. 2025. PMID: 39514161
References
-
- Wilmot EG, Edwardson CL, Achana FA, Davies MJ, Gorely T, Gray LJ, Khunti K, Yates T, Biddle SJ. Sedentary time in adults and the association with diabetes, cardiovascular disease and death: systematic review and meta-analysis. Diabetologia. 2012;55:2895–2905. doi: 10.1007/s00125-012-2677-z. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

