High level of persister frequency in clinical staphylococcal isolates
- PMID: 35448965
- PMCID: PMC10124895
- DOI: 10.1186/s12866-022-02529-7
High level of persister frequency in clinical staphylococcal isolates
Abstract
Background: Staphylococcus aureus is a notorious human pathogen that causes often lethal systemic conditions that are mostly medical device associated biofilm infections. Similarly, coagulase negative staphylococci are emerging as leading pathogen for nosocomial infections owing to their ability to form biofilm on implanted medical equipment. Chronic in nature, these infections are difficult to treat. Such recalcitrance of these infections is caused mainly due to the presence of persister cells, which exhibit transient yet extreme tolerance to antibiotics. Despite tremendous clinical significance, there is lack of studies on persister cells formation among clinical bacterial isolates. Considering the importance of factors influencing persister formation, in this study, we evaluate the association of antibiotic tolerance with biofilm production, antibiotic stress, growth phase, specimen type, and dependency on staphylococcal species. Biofilm formation was detected among 375 clinical staphylococcal isolates by quantitative tissue culture plate method (TCP) and icaAD genes by genotypic method. The antibiotic susceptibility was determined by Kirby Bauer disc diffusion method while minimum inhibitory concentration values were obtained by agar dilution method. Persister cells were measured in the susceptible staphylococcal isolates in the presence of clinically relevant antibiotics.
Results: In the study, 161 (43%) S. aureus and 214 (57%) coagulase negative staphylococci (CNS) were isolated from different clinical samples. TCP method detected biofilm production in 84 (52.2%) S. aureus and 90 (42.1%) CNS isolates. The genotypic method detected icaAD genes in 86 (22.9%) isolates. Majority (> 90%) of both the biofilm producers and non-producers were sensitive to chloramphenicol and tetracycline but were resistant to penicillin. Interestingly, all isolates were sensitive to vancomycin irrespective of biofilm production. While high persister frequency was observed among all staphylococci isolates in the stationary growth phase, the persister frequency in exponential growth phase was statistically high among isolates possessing icaAD genes compared to icaAD negative isolates.
Conclusion: The research findings provide strong evidence that the clinical staphylococcal isolates exhibit extreme antibiotic tolerance suggesting their causal link with treatment failures. Understanding the factors influencing the formation and maintenance of persister cells are of utmost important aspect to design therapeutics and control recalcitrant bacterial infections.
Keywords: Biofilm; Clinical staphylococcal isolates; Persister cells; icaAD genes.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

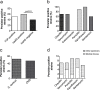
References
-
- Bigger JW. Treatment of Staphylococcal infections with penicillin by intermittant sterilisation. Lancet Infect Dis. 1944;244:4.
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

