CT review of ovarian fibrothecoma
- PMID: 35451310
- PMCID: PMC10162058
- DOI: 10.1259/bjr.20210790
CT review of ovarian fibrothecoma
Abstract
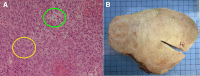
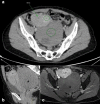
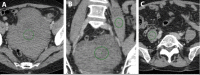
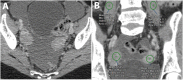
Objective: The aim of this study was to investigate the CT imaging characteristics of ovarian fibrothecoma which may aid in the differentiation from early stage epithelial tumours.
Methods: Comparison of 36 patients (41 lesions) with pathologically proven ovarian fibrothecoma tumours and 36 (52 lesions) serous papillary carcinomas (SPCs) lesions. We noted their laterality, size, density, calcifications, Hounsfield units (HUs) and introduced a novel HU comparison technique with the psoas muscle or the uterus. Patients' clinical findings such as ascites, pleural effusion, carbohydrate antigen-125 levels, and lymphadenopathy findings were also included.
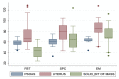
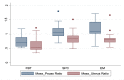
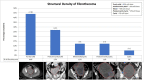
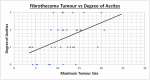
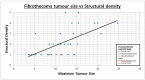
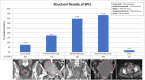
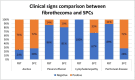
Results: Average age was 67.8 and 66 across the fibrothecoma and SPC cohort respectively. Fibrothecoma tumours had diameters ranging from 24 to 207 mm (Median: 94 mm). 80.6% of the fibrothecoma cohort had ascites which was comparable to the 72.2% in the SPC cohort. 70.7% of fibrothecoma tumour favour a purely to predominantly solid structural configuration (p < 0.001). The average HU value for the fibrothecoma solid component was 44 ± 11.7 contrasting the SPC HU value of 66.8 ± 15. The psoas:tumour mass ratio demonstrated a median of 0.7, whereas SPCs shows a median of 1.1 (p < 0.001).
Conclusion: Suspicion of ovarian fibrothecoma should be considered through interrogation of their structural density configuration, low psoas to mass HU ratio and a presence of ascites.
Advances in knowledge: CT imaging can be a useful tool in diagnosing fibrothecoma tumours and subsequently reducing oncogynaecological tertiary centre referrals, financial burden and patient operative morbidity and mortality.
Figures
References
-
- Kurman RJ RJ, Carcangiu ML ML, Herrington C. Classification of tumours of the ovary. 4th ed. WHO Classification of Tumours; 2014, pp.44–56.
MeSH terms
Substances
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical

