Sleep Disturbance and Quality of Life in Rheumatoid Arthritis: Prospective mHealth Study
- PMID: 35451978
- PMCID: PMC9077504
- DOI: 10.2196/32825
Sleep Disturbance and Quality of Life in Rheumatoid Arthritis: Prospective mHealth Study
Abstract
Background: Sleep disturbances and poor health-related quality of life (HRQoL) are common in people with rheumatoid arthritis (RA). Sleep disturbances, such as less total sleep time, more waking periods after sleep onset, and higher levels of nonrestorative sleep, may be a driver of HRQoL. However, understanding whether these sleep disturbances reduce HRQoL has, to date, been challenging because of the need to collect complex time-varying data at high resolution. Such data collection is now made possible by the widespread availability and use of mobile health (mHealth) technologies.
Objective: This mHealth study aimed to test whether sleep disturbance (both absolute values and variability) causes poor HRQoL.
Methods: The quality of life, sleep, and RA study was a prospective mHealth study of adults with RA. Participants completed a baseline questionnaire, wore a triaxial accelerometer for 30 days to objectively assess sleep, and provided daily reports via a smartphone app that assessed sleep (Consensus Sleep Diary), pain, fatigue, mood, and other symptoms. Participants completed the World Health Organization Quality of Life-Brief (WHOQoL-BREF) questionnaire every 10 days. Multilevel modeling tested the relationship between sleep variables and the WHOQoL-BREF domains (physical, psychological, environmental, and social).
Results: Of the 268 recruited participants, 254 were included in the analysis. Across all WHOQoL-BREF domains, participants' scores were lower than the population average. Consensus Sleep Diary sleep parameters predicted the WHOQoL-BREF domain scores. For example, for each hour increase in the total time asleep physical domain scores increased by 1.11 points (β=1.11, 95% CI 0.07-2.15) and social domain scores increased by 1.65 points. These associations were not explained by sociodemographic and lifestyle factors, disease activity, medication use, anxiety levels, sleep quality, or clinical sleep disorders. However, these changes were attenuated and no longer significant when pain, fatigue, and mood were included in the model. Increased variability in total time asleep was associated with poorer physical and psychological domain scores, independent of all covariates. There was no association between actigraphy-measured sleep and WHOQoL-BREF.
Conclusions: Optimizing total sleep time, increasing sleep efficiency, decreasing sleep onset latency, and reducing variability in total sleep time could improve HRQoL in people with RA.
Keywords: HRQoL; QoL; WHOQoL-BREF; fatigue; health-related quality of life; mobile health; mobile phone; mood; pain; quality of life; rheumatoid arthritis; sleep; sleep disturbance; sleep efficiency.
©John McBeth, William G Dixon, Susan Mary Moore, Bruce Hellman, Ben James, Simon D Kyle, Mark Lunt, Lis Cordingley, Belay Birlie Yimer, Katie L Druce. Originally published in the Journal of Medical Internet Research (https://www.jmir.org), 22.04.2022.
Conflict of interest statement
Conflicts of Interest: WGD has received consultancy fees from Google and Abbvie (unrelated to this work).
Figures
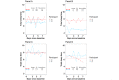
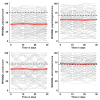
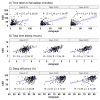
References
-
- Dominick KL, Ahern FM, Gold CH, Heller DA. Health-related quality of life among older adults with arthritis. Health Qual Life Outcomes. 2004 Jan 13;2:5. doi: 10.1186/1477-7525-2-5. https://hqlo.biomedcentral.com/articles/10.1186/1477-7525-2-5 1477-7525-2-5 - DOI - DOI - PMC - PubMed
-
- Roehrs T, Diederichs C, Gillis M, Burger AJ, Stout RA, Lumley MA, Roth T. Nocturnal sleep, daytime sleepiness and fatigue in fibromyalgia patients compared to rheumatoid arthritis patients and healthy controls: a preliminary study. Sleep Med. 2013 Jan;14(1):109–15. doi: 10.1016/j.sleep.2012.09.020.S1389-9457(12)00369-3 - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

