Parenchymal Insults in Abuse-A Potential Key to Diagnosis
- PMID: 35454003
- PMCID: PMC9029348
- DOI: 10.3390/diagnostics12040955
Parenchymal Insults in Abuse-A Potential Key to Diagnosis
Abstract
Subdural hemorrhage is a key imaging finding in cases of abusive head trauma and one that many radiologists and radiology trainees become familiar with during their years of training. Although it may prove to be a marker of trauma in a young child or infant that presents without a history of injury, the parenchymal insults in these young patients more often lead to the debilitating and sometimes devastating outcomes observed in this young population. It is important to recognize these patterns of parenchymal injuries and how they may differ from the imaging findings in other cases of traumatic injury in young children. In addition, these parenchymal insults may serve as another significant, distinguishing feature when making the medical diagnosis of abusive head injury while still considering alternative diagnoses, including accidental injury. Therefore, as radiologists, we must strive to look beyond the potential cranial injury or subdural hemorrhage for the sometimes more subtle but significant parenchymal insults in abuse.
Keywords: abusive head trauma; child abuse; computed tomography; hypoxic-ischemic injury; magnetic resonance imaging.
Conflict of interest statement
The author declares no conflict of interest.
Figures
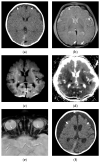
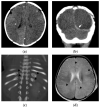

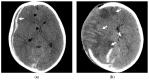
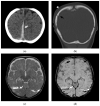
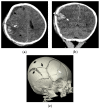
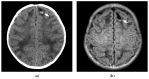

Similar articles
-
Usefulness of MRI detection of cervical spine and brain injuries in the evaluation of abusive head trauma.Pediatr Radiol. 2014 Jul;44(7):839-48. doi: 10.1007/s00247-014-2874-7. Epub 2014 Feb 21. Pediatr Radiol. 2014. PMID: 24557483
-
Various Cranial and Orbital Imaging Findings in Pediatric Abusive and Non-abusive Head trauma, and Relation to Outcomes.Clin Neuroradiol. 2019 Jun;29(2):253-261. doi: 10.1007/s00062-018-0663-7. Epub 2018 Jan 23. Clin Neuroradiol. 2019. PMID: 29362831
-
Spinal subdural hemorrhage in abusive head trauma: a retrospective study.Radiology. 2012 Jan;262(1):216-23. doi: 10.1148/radiol.11102390. Epub 2011 Nov 8. Radiology. 2012. PMID: 22069156
-
Imaging abusive head trauma: why use both computed tomography and magnetic resonance imaging?Pediatr Radiol. 2014 Dec;44 Suppl 4:S589-603. doi: 10.1007/s00247-014-3216-5. Epub 2014 Dec 14. Pediatr Radiol. 2014. PMID: 25501731 Review.
-
Pediatric Central Nervous System Imaging of Nonaccidental Trauma: Beyond Subdural Hematomas.Radiographics. 2019 Jan-Feb;39(1):213-228. doi: 10.1148/rg.2019180084. Epub 2018 Nov 23. Radiographics. 2019. PMID: 30468627 Review.
Cited by
-
Benign enlargement of the subarachnoid spaces and subdural collections-when to evaluate for abuse.Pediatr Radiol. 2023 Apr;53(4):752-767. doi: 10.1007/s00247-023-05611-y. Epub 2023 Mar 1. Pediatr Radiol. 2023. PMID: 36856756 Free PMC article.
-
Spectrum of Magnetic Resonance Imaging Findings in Acute Pediatric Traumatic Brain Injury - A Pictorial Essay.J Multidiscip Healthc. 2024 Jun 19;17:2921-2934. doi: 10.2147/JMDH.S466044. eCollection 2024. J Multidiscip Healthc. 2024. PMID: 38911614 Free PMC article. Review.
References
-
- U.S. Department of Health and Human Services, AfCaF Child Welfare Information Gateway. Child Abuse and Neglect Fatalities 2019: Statistics and Interventions. [(accessed on 28 February 2022)];2021 Available online: https://www.childwelfare.gov/pubs/factsheets/fatality/
-
- Choudhary A.K., Servaes S., Slovis T.L., Palusci V.J., Hedlund G.L., Narang S.K., Moreno J.A., Dias M.S., Christian C.W., Nelson M.D., Jr., et al. Consensus statement on abusive head trauma in infants and young children. Pediatr. Radiol. 2018;48:1048–1065. doi: 10.1007/s00247-018-4149-1. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

