Hepatectomy or/with Metastatectomy for Recurrent Intrahepatic Cholangiocarcinoma: Of Promise for Selected Patients
- PMID: 35455657
- PMCID: PMC9029635
- DOI: 10.3390/jpm12040540
Hepatectomy or/with Metastatectomy for Recurrent Intrahepatic Cholangiocarcinoma: Of Promise for Selected Patients
Abstract
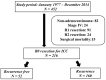
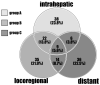
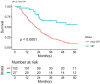
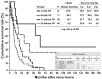
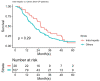
Introduction: Intrahepatic cholangiocarcinoma (ICC) has devastating outcomes owing to its advanced stage at diagnosis and high recurrence after hepatectomy. There is no preferred treatment for recurrent ICC. We retrospectively reviewed our patients who underwent repeated operations for recurrent ICCs based on their different indications to appraise the outcomes. Methods: In all, 160 out of 216 patients with ICC (71.4%) experienced recurrence after curative resection from 1977 to 2014. The patterns of recurrence were categorized according to the locations and numbers of recurrent tumors. Results: Patients with merely intrahepatic recurrence (n = 38) had superior overall survival (OS) compared with those with beyond intrahepatic recurrence (p < 0.0001). Twenty-seven out of 160 patients (16.8%) underwent repeat hepatectomy or/with metastatectomy for recurrence and had superior OS when compared to the remaining 133 patients who received nonoperative treatment/palliation (85.6 months versus 20.9 months, p < 0.001). Furthermore, patients suitable for repeat hepatectomy in the intrahepatic recurrent group (n = 12) had superior post-recurrence overall survival (PROS) than the remaining 26 patients receiving nonoperative treatment (61.6 months versus 14.7 months, p < 0.05). Conclusion: Liver is the most commonly involved site of recurrent ICC. However, merely intrahepatic recurrence may have a favorable prognosis compared to recurrence involving other sites. Aggressive hepatectomy may provide a survival benefit in selected patients.
Keywords: hepatectomy; intrahepatic cholangiocarcinoma; metastatectomy; overall survival; recurrent intrahepatic cholangiocarcinoma.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures


References
-
- Nakeeb A., Pitt H.A., Sohn T.A., Coleman J., Abrams R.A., Piantadosi S., Hruban R.H., Lillemoe K.D., Yeo C.J., Cameron J.L. Cholangiocarcinoma. A spectrum of intrahepatic, perihilar, and distal tumors. Ann. Surg. 1996;224:463–473. doi: 10.1097/00000658-199610000-00005. discussion 473–475. - DOI - PMC - PubMed
-
- DeOliveira M.L., Cunningham S.C., Cameron J.L., Kamangar F., Winter J.M., Lillemoe K.D., Choti M.A., Yeo C.J., Schulick R.D. Cholangiocarcinoma: Thirty-one-year experience with 564 patients at a single institution. Ann. Surg. 2007;245:755–762. doi: 10.1097/01.sla.0000251366.62632.d3. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

