Long-Term Analysis of Resilience of the Oral Microbiome in Allogeneic Stem Cell Transplant Recipients
- PMID: 35456787
- PMCID: PMC9030553
- DOI: 10.3390/microorganisms10040734
Long-Term Analysis of Resilience of the Oral Microbiome in Allogeneic Stem Cell Transplant Recipients
Abstract
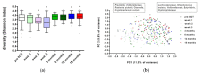
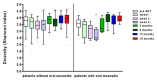
Stem cell transplantation (SCT) is associated with oral microbial dysbiosis. However, long-term longitudinal data are lacking. Therefore, this study aimed to longitudinally assess the oral microbiome in SCT patients and to determine if changes are associated with oral mucositis and oral chronic graft-versus-host disease. Fifty allogeneic SCT recipients treated in two Dutch university hospitals were prospectively followed, starting at pre-SCT, weekly during hospitalization, and at 3, 6, 12, and 18 months after SCT. Oral rinsing samples were taken, and oral mucositis (WHO score) and oral chronic graft-versus-host disease (NIH score) were assessed. The oral microbiome diversity (Shannon index) and composition significantly changed after SCT and returned to pre-treatment levels from 3 months after SCT. Oral mucositis was associated with a more pronounced decrease in microbial diversity and with several disease-associated genera, such as Mycobacterium, Staphylococcus, and Enterococcus. On the other hand, microbiome diversity and composition were not associated with oral chronic graft-versus-host disease. To conclude, dysbiosis of the oral microbiome occurred directly after SCT but recovered after 3 months. Diversity and composition were related to oral mucositis but not to oral chronic graft-versus-host disease.
Keywords: allogeneic stem cell transplant; conditioning; dysbiosis; oral graft-versus-host disease; oral microbiome; oral mucositis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures




References
Grants and funding
LinkOut - more resources
Full Text Sources

