Use of metallic and polymeric ureteral stents in malignant ureteral obstruction
- PMID: 35474665
- PMCID: PMC8988829
- DOI: 10.1002/bco2.51
Use of metallic and polymeric ureteral stents in malignant ureteral obstruction
Abstract
Background: Malignant ureteral obstruction (MUO) is often caused by advanced intra-abdominal cancers. Effective management must be attempted, but the treatment policy is unclear. Metallic ureteral stents are one of the latest options in managing MUO. Metallic ureteral stents are superior to traditional polyurethane stents. The present study retrospectively reviewed our four institutions' experiences with treating MUO using metallic ureteral stent.
Methods: A total of 45 patients who required metallic ureteral stent placement for MUO at Yokohama City University Medical Center (Yokohama, JAPAN) between January 2014 and May 2016 were analyzed. We defined stent failure as having to change the ureteral stent before the scheduled ureteral stent exchange time or having to perform percutaneous nephrostomy (PCN). Complications were defined as an unscheduled hospital visit or hospitalization caused by incompatibility, infection, and pain of the metallic ureteral stent, etc., unrelated to the primary disease. We compared stent failure and the overall survival (OS) between metallic and polymeric ureteral stents. To evaluate the workload of the medical staff, we used the NASA Task Load Index (NASA-TLX) in a total of 11 urologists.
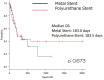
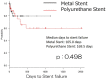
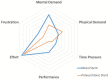
Results: During the observation period, 8 (17.8%) patients in the metallic ureteral stent group and 10 (27.8%) in the control group developed stent failure. Complications were noted in 14 (31.1%) patients in the metallic ureteral stent group and 15 (41.7%) patients in the control group. A Kaplan-Meier analysis and log-rank test showed no significant differences between two groups in the overall survival (P = 0.673). One or more complications developed in 19 (32.2%) patients in the metallic ureteral stent group and 18 (38.3%) patients in the control group (P = 0.409). Renal dysfunction after the replacement of the ureteral stent developed in 9 (15.3%) patients in the metallic ureteral stent group and 14 (29.8%) patients in the control group. No patients developed a urinary tract infection (UTI) that required hospitalization in the metallic ureteral stent group, whereas 3 (6.4%) patients in the control group had a UTI that was treated with hospitalization. The average workload score in the six subscales was analyzed, and the scores for mental demand and performance were higher in the metallic ureteral stent group, although there was no significant difference between the metallic and polymeric ureteral stent groups.
Conclusions: Metallic ureteral stents showed favorable ureteral stent patency and reduced the workload for urologists.
Keywords: malignant ureteral obstruction; ureteral stenting.
© 2020 The Authors. BJUI Compass published by John Wiley & Sons Ltd on behalf of BJU International Company.
Conflict of interest statement
We declare no conflicts of interest.
Figures
References
-
- Abt D, Warzinek E, Schmid HP, Haile SR, Engeler DS. Influence of patient education on morbidity caused by ureteral stents. Int J Urol. 2015;22(7):679–83. - PubMed
-
- Elsamra SE, Leavitt DA, Motato HA, Friedlander JI, Siev M, Keheila M, et al. Stenting for malignant ureteral obstruction: tandem, metal or metal‐mesh stents. Int J Urol. 2015;22(7):629–36. - PubMed
-
- Rosenberg BH, Bianco FJ Jr, Wood DP Jr, Triest JA. Stent‐change therapy in advanced malignancies with ureteral obstruction. J Endourol. 2005;19(1):63–7. - PubMed
-
- Yossepowitch O, Lifshitz DA, Dekel Y, Gross M, Keidar DM, Neuman M, et al. Predicting the success of retrograde stenting for managing ureteral obstruction. J Urol. 2001;166(5):1746–9. - PubMed
LinkOut - more resources
Full Text Sources