Transperineal prostate biopsy identifies locations of clinically significant prostate cancer in men considering focal therapy with PI-RADS 3-5 regions of interest
- PMID: 35474703
- PMCID: PMC8988820
- DOI: 10.1002/bco2.111
Transperineal prostate biopsy identifies locations of clinically significant prostate cancer in men considering focal therapy with PI-RADS 3-5 regions of interest
Abstract
Objectives: To determine the benefit of performing transperineal prostate mapping biopsy (TPMB) following multiparametric magnetic resonance imaging (mpMRI) to increase the identification of clinically significant prostate cancer (csPCa) with Gleason grade group (GG) ≥ 2 and their locations outside of the PI-RADS v2 3-5 category lesions.
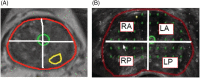
Methods: mpMRI was performed in 80 men prior TPMB from two institutions. The mpMRI was considered clinically significant (csMRI) if it contained one or more PI-RADS 3-5 category lesion. mpMRI findings were compared against csPCa diagnosed by TPMB, performed between 16 November 2010, and 13 September 2019, for the entire gland, both lobes and to the right and left anterior and right and left posterior quadrants (RA, LA, RP and LP). Sensitivity, specificity, positive and negative predictive values (PPV, NPV), accuracy and the area under curve (AUC) were determined. Thirteen men also underwent radical prostatectomy and had comparison of TPMB pathology to prostatectomy specimen grading.
Results: TPMB was positive in 60/80 (75%) of which 32 (53.3%) were csPCa. csPCa was present in the RA in 9 (11.3%), LA in 11 (13.8%), RP in 25 (31.3%) and LP in 27 (33.8%) and involved 1 quadrant in 7 (21.9%), 2 quadrants in 12 (37.5%), 3 quadrants in 11 (34.4%) and all 4 quadrants in 2 (6.3%) patients; 57/80 (71.3%) men had a mpMRIs with lesions designated as PI-RADS 3 in 24 (30%), 4 in 25 (31.3%) and 5 in 8 (10%). A csMRI was present in the RA in 7 (8.8%), LA in 8 (10%), RP in 31 (38.8%) and in the LP in 29 (36.3%), which were limited to one quadrant in 39 (68.4%), 2 quadrants in 16 (28.1%), and 3 quadrants in 2 (3.5%). Sensitivity, specificity, PPV, and NPV were determined from the results of the TPMB and were for the entire gland 81.3%, 35.4%, 45.6% and 73.9%. There were 31 csMRIs involving the right posterior of the gland but only 25 csPCa by TPMB of which 12/31 (38.7%) were concordant for high grade disease. There were 29 men who have a csMRI in the left posterior quadrant, and 14 (48.3%) were concordant with csPCa from the TPMB.
Conclusions: MpMRI should be supplemented with TPMB to correctly identify the regions of the prostate that would require ablation in men considering focal therapy.
Keywords: mpMRI; prostate biopsy; transperineal mapping.
© 2021 The Authors. BJUI Compass published by John Wiley & Sons Ltd on behalf of BJU International Company.
Conflict of interest statement
N. N. Stone and M. S. Lucia have ownerships in Triopsy, Inc. There was no financial assistance from Triopsy in this investigation or in the production of the manuscript.
Figures
Similar articles
-
Association Between Prostate Imaging Reporting and Data System (PI-RADS) Score for the Index Lesion and Multifocal, Clinically Significant Prostate Cancer.Eur Urol Oncol. 2018 May;1(1):29-36. doi: 10.1016/j.euo.2018.01.002. Epub 2018 May 15. Eur Urol Oncol. 2018. PMID: 31100225
-
Assessment of PI-RADS v2 categories ≥ 3 for diagnosis of clinically significant prostate cancer.Abdom Radiol (NY). 2019 Feb;44(2):705-712. doi: 10.1007/s00261-018-1751-5. Abdom Radiol (NY). 2019. PMID: 30171296
-
The diagnostic accuracy of multiparametric magnetic resonance imaging before biopsy in the detection of prostate cancer.BJU Int. 2019 Jan;123(1):82-90. doi: 10.1111/bju.14420. Epub 2018 Jul 26. BJU Int. 2019. PMID: 29804315
-
Evaluation of the accuracy of multiparametric MRI for predicting prostate cancer pathology and tumour staging in the real world: an multicentre study.BJU Int. 2019 Aug;124(2):297-301. doi: 10.1111/bju.14696. Epub 2019 Feb 25. BJU Int. 2019. PMID: 30714285
-
Multiparametric Magnetic Resonance Imaging in the Diagnosis of Clinically Significant Prostate Cancer: an Updated Systematic Review.Clin Oncol (R Coll Radiol). 2021 Dec;33(12):e599-e612. doi: 10.1016/j.clon.2021.07.016. Epub 2021 Aug 13. Clin Oncol (R Coll Radiol). 2021. PMID: 34400038
Cited by
-
Method to determine the nadir PSA following partial gland ablation.BJUI Compass. 2025 Feb 14;6(2):e496. doi: 10.1002/bco2.496. eCollection 2025 Feb. BJUI Compass. 2025. PMID: 39958259 Free PMC article.
-
BJUI Compass 2021 year-end review.BJUI Compass. 2021 Nov 17;2(6):357-358. doi: 10.1002/bco2.122. eCollection 2021 Nov. BJUI Compass. 2021. PMID: 35474699 Free PMC article. No abstract available.
References
-
- Patel NU, Lind KE, Garg K, Crawford D, Werahera PN, Pokharel SS. Assessment of PI‐RADS v2 categories >/= 3 for diagnosis of clinically significant prostate cancer. Abdom Radiol. 2019;44:705–12. - PubMed
-
- Sathianathen NJ, Omer A, Harriss E, Davies L, Kasivisvanathan V, Punwani S, et al. Negative predictive value of multiparametric magnetic resonance imaging in the detection of clinically significant prostate Cancer in the prostate imaging reporting and data system era: a systematic review and Meta‐analysis. Eur Urol. 2020;78:402–14. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
