Multiple recurrences of unknown primary tumor in a meningioma: A case report
- PMID: 35488191
- PMCID: PMC9626840
- DOI: 10.1177/19714009221096836
Multiple recurrences of unknown primary tumor in a meningioma: A case report
Abstract
Metastasis of a systemic tumor into a primary brain tumor has been rarely reported in the literature. These metastases could be seen mostly in meningiomas and in less frequently in the other intracranial tumors. Carcinoma of an unknown primary site (CUP) metastasizing into an intracranial meningioma is not a common occasion. According to the best of our knowledge, in this report, we present the first case with multiple recurrent CUP, which metastasized to intracranial meningioma, reported in the literature. The whole body was investigated with FDG PET/CT and biomarkers of the most common carcinomas for primary cancer. However, these tests showed no primary affected region. Despite all adjuvant therapies, the tumor had multiple recurrences. Such cases are still a challenge to offer optimal management.
Keywords: Brain metastasis; meningioma; primary unknown metastasis.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
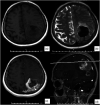
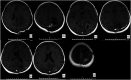

References
-
- Lanotte M, Benech F, Panciani PP, et al. Systemic cancer metastasis in a meningioma: report of two cases and review of the literature. Clin Neurol Neurosurg 2009; 111(1): 87–93. - PubMed
-
- Benedetto N, Perrini P, Scollato A, et al. Intracranial meningioma containing metastatic colon carcinoma. Acta Neurochirurgica 2007; 149(8): 799–803. - PubMed
-
- Chambers PW, Davis RL, Blanding JD, et al. Metastases to primary intracranial meningiomas and neurilemomas. Arch Pathol Lab Med 1980; 104: 350–354. - PubMed
-
- Lodrini S, Savoiardo M. Metastases of carcinoma to intracranial meningioma: report of two cases and review of the literature. Cancer 1981; 48: 2668–2673. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

