LEARN: A multi-centre, cross-sectional evaluation of Urology teaching in UK medical schools
- PMID: 35488402
- PMCID: PMC9796355
- DOI: 10.1111/bju.15758
LEARN: A multi-centre, cross-sectional evaluation of Urology teaching in UK medical schools
Abstract
Objective: To evaluate the status of UK undergraduate urology teaching against the British Association of Urological Surgeons (BAUS) Undergraduate Syllabus for Urology. Secondary objectives included evaluating the type and quantity of teaching provided, the reported performance rate of General Medical Council (GMC)-mandated urological procedures, and the proportion of undergraduates considering urology as a career.
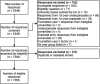
Materials and methods: LEARN was a national multicentre cross-sectional study. Year 2 to Year 5 medical students and FY1 doctors were invited to complete a survey between 3rd October and 20th December 2020, retrospectively assessing the urology teaching received to date. Results are reported according to the Checklist for Reporting Results of Internet E-Surveys (CHERRIES).
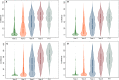
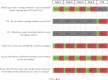
Results: 7,063/8,346 (84.6%) responses from all 39 UK medical schools were included; 1,127/7,063 (16.0%) were from Foundation Year (FY) 1 doctors, who reported that the most frequently taught topics in undergraduate training were on urinary tract infection (96.5%), acute kidney injury (95.9%) and haematuria (94.4%). The most infrequently taught topics were male urinary incontinence (59.4%), male infertility (52.4%) and erectile dysfunction (43.8%). Male and female catheterisation on patients as undergraduates was performed by 92.1% and 73.0% of FY1 doctors respectively, and 16.9% had considered a career in urology. Theory based teaching was mainly prevalent in the early years of medical school, with clinical skills teaching, and clinical placements in the later years of medical school. 20.1% of FY1 doctors reported no undergraduate clinical attachment in urology.
Conclusion: LEARN is the largest ever evaluation of undergraduate urology teaching. In the UK, teaching seemed satisfactory as evaluated by the BAUS undergraduate syllabus. However, many students report having no clinical attachments in Urology and some newly qualified doctors report never having inserted a catheter, which is a GMC mandated requirement. We recommend a greater emphasis on undergraduate clinical exposure to urology and stricter adherence to GMC mandated procedures.
Keywords: Urology; clinical skills; education; medical students; teaching; undergraduate; urology curriculum..
This article is protected by copyright. All rights reserved.
Figures
References
-
- NHS England . NHS Workforce Statistics – December 2020 (Including selected provisional statistics for January 2021) – NHS Digital. 2021. Available at: https://digital.nhs.uk/data‐and‐information/publications/statistical/nhs.... Accessed 24 April 2021
-
- Hashim H, Jones P, Flynn KJO, Pearce I, Royle J, Shaw M et al. An Undergraduate Syllabus for Urology. Br Assoc Urol Surg. 2012; 1–7 Available at: https://www.baus.org.uk/_userfiles/pages/files/professionals/education/U.... Accessed 30 March 2020
-
- DRM Smith, Pouwels KB, Hopkins S, Naylor NR, Smieszek T, Robotham JV. Epidemiology and health‐economic burden of urinary‐catheter‐associated infection in English NHS hospitals: a probabilistic modelling study. 2019. Available at: www.sciencedirect.com. Accessed 5 July 2021 - PubMed
-
- Ng A, Light A, VWS C, Asif A, Bhatt NR, Kasivisvanathan V. Urology teaching in UK medical schools: does it prepare doctors adequately? Nat Rev Urol 2020; 17: 651–2 - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

