Impact of prelacteal feeds and neonatal introduction of breast milk substitutes on breastfeeding outcomes: A systematic review and meta-analysis
- PMID: 35489107
- PMCID: PMC9113480
- DOI: 10.1111/mcn.13368
Impact of prelacteal feeds and neonatal introduction of breast milk substitutes on breastfeeding outcomes: A systematic review and meta-analysis
Abstract
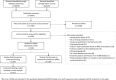
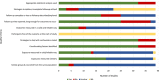
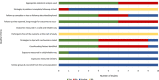
The introduction of fluids other than breast milk during the first few days of life or later neonatal period has been identified as a risk factor for suboptimal breastfeeding (BF) outcomes in numerous studies using varying study designs. However, the relationship between early introduction of fluids other than breast milk and BF outcomes has not been systematically assessed using only prospective studies that can establish temporality, which is critical for determining whether observed associations are causal. We conducted a systematic review and meta-analysis of prospective studies to assess if there is a difference in BF outcomes as a result of the introduction of: (a) milk-based prelacteals, (b) water-based prelacteals and (c) breast milk substitutes (BMS) between 4 days and 4 weeks postpartum. We searched PubMed, Lilacs, Web of Science and other repositories for original research investigating the relationship between early introduction of prelacteals and/or BMS and BF outcomes. Forty-eight studies met the inclusion criteria for the systematic review. Of the 39 prelacteal feeding studies, 27 had the prerequisite statistical information for inclusion in the meta-analysis. Findings from the meta-analysis showed a relationship between prelacteals and exclusive BF cessation (RR 1.44; 1.29-1.60) and any BF cessation (2.23; 1.63-3.06) among infants under 6 months old. Nine studies focusing on the introduction of BMS during the neonatal period identified this practice as a statistically significant risk factor for a shorter BF duration. Effective interventions are needed to prevent the introduction of unnecessary milk-based prelacteals and BMS during the perinatal and neonatal periods to improve BF outcomes.
Keywords: breast milk substitutes; breastfeeding; infant feeding; meta-analysis; neonatal period; prelacteal feeds.
© 2022 The Authors. Maternal & Child Nutrition published by John Wiley & Sons Ltd.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures



References
-
- Alikasifoglu, M. , Erginoz, E. , Gur, E. T. , Baltas, Z. , Beker, B. , & Arvas, A. (2001). Factors influencing the duration of exclusive breastfeeding in a group of Turkish women. Journal of Human Lactation: Official Journal of International Lactation Consultant Association, 17(3), 220–226. - PubMed
-
- Barría, M. , Orozco, B. , Gatica, M. , Mackenney, J. , Valverde, C. , Drago, M. , & Valencia, C. (1990). [Early introduction of dairy formulas in infant feeding]. Revista Chilena de Pediatria, 61(4), 218–222. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

