Maximum subjective outcome improvement is reported by 3 Months following arthroscopic partial meniscectomy: A systematic review
- PMID: 35496357
- PMCID: PMC9043384
- DOI: 10.1016/j.jor.2022.04.007
Maximum subjective outcome improvement is reported by 3 Months following arthroscopic partial meniscectomy: A systematic review
Abstract
Purpose: To review patient outcomes in the literature following arthroscopic partial meniscectomy (APM) in order to identify when patients report reaching subjective maximal improvement postoperatively.
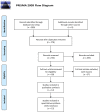
Methods: A systematic review of the literature from January 2004 to August 2019 was conducted using PRISMA guidelines to identify articles evaluating patient-reported outcome measures (PROMs) up to a minimum of 6 months after APM in patients >18 years old. Studies were excluded if additional interventions were performed such as repairs, ligamentous reconstruction or repair, cartilaginous manipulation, or revision surgery. PROMs were pooled between studies at preoperative, 3 months, 6 months, 1 year, and 2 year time points. Weighted averages were used within a mixed model method in order to account for the differences in sample size and variance among studies. Significant improvements in PROMs at various time intervals were statistically analyzed using minimal clinically important difference.
Results: A total of 12 studies including 1663 patients who underwent APM were selected for the review. The pooled cohort consisted of 1033 (62%) males and 630 (38%) females. Significant improvements were demonstrated from preoperative scores to 3 months postoperatively in Knee Injury and Osteoarthritis Outcome Score subcategories, Lysholm, and visual analog scale scores while no differences were found for Tegner and International Knee Documentation Committee scores. Although statistically significant improvement in PROMs remained at all postoperative time points compared to preoperative scores, no significant differences were observed after 3 months postoperatively.
Conclusions: Patients undergoing APM had significant mean changes in legacy PROMs by 3 months postoperatively that exceeded given minimal clinically important difference values, without further clinically important improvement reported up to 2 years postoperatively.
Study design: Level III, systematic review.
Keywords: Arthroscopic; Knee; Maximal medical improvement; Meniscal tear; Meniscectomy; Meniscus; Patient-reported outcome measures.
© 2022 Professor P K Surendran Memorial Education Foundation. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
K.R.O. has received grant support from Arthrex; education payments from Arthrex, Medwest, and Smith & Nephew; consulting fees from Endo Pharmaceuticals and Smith & Nephew; nonconsulting fees from Arthrex; and hospitality payments from Stryker, Wright Medical, and Zimmer Biomet. All other authors have no financial disclosures.
Figures
References
-
- Raj M.A., Bubnis M.A. StatPearls Publishing; Island, FL: 2021. Knee Meniscal Tears. StatPearls. Treasure. NBK431067. - PubMed
-
- Kurzweil P.R., Cannon W.D., DeHaven K.E. Meniscus repair and replacement. Sports Med Arthrosc Rev. 2018;26:160–164. - PubMed
-
- van de Graaf V.A., Wolterbeek N., Mutsaerts E.L., et al. Arthroscopic partial meniscectomy or conservative treatment for nonobstructive meniscal tears: a systematic review and meta-analysis of randomized controlled trials. Arthroscopy. 2016;32:1855–1865. the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association, e1854. - PubMed
-
- Baker B.E., Peckham A.C., Pupparo F., Sanborn J.C. Review of meniscal injury and associated sports. Am J Sports Med. 1985;13:1–4. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

