Effect of Systemic Lidocaine on Postoperative Early Recovery Quality in Patients Undergoing Supratentorial Tumor Resection
- PMID: 35496368
- PMCID: PMC9041358
- DOI: 10.2147/DDDT.S359755
Effect of Systemic Lidocaine on Postoperative Early Recovery Quality in Patients Undergoing Supratentorial Tumor Resection
Abstract
Purpose: Lidocaine has been gradually used in general anesthesia. This study was designed to investigate the effect of systemic lidocaine on postoperative quality of recovery (QoR) in patients undergoing supratentorial tumor resection, and to explore its brain-injury alleviation effect in neurosurgical anesthesia.
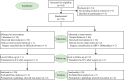
Patients and methods: Sixty adult patients undergoing elective supratentorial tumor resection. Patients were randomly assigned either to receive lidocaine (Group L: 1.5 mg/kg bolus completed 10 min before anesthesia induction followed by an infusion at 2.0 mg/kg/h) or to receive normal saline (Group C: received volume-matched normal saline at the same infusion rate). Primary outcome measures were Quality of Recovery-40 (QoR-40) scores on postoperative day (POD) 1 and 2. Plasma concentrations of S100B protein (S100B), neuron specific enolase (NSE), interleukin-6 (IL-6) and tumor necrosis factor-α (TNF-α) before anesthesia induction and at the end of surgery were assessed. Visual Analogue Scale (VAS) scores were assessed at 1, 2, 6, 12, 24 and 48 h after surgery. Perioperative parameters and adverse events were also recorded.
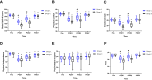
Results: Patients between two groups had comparable baseline characteristics. Global QoR-40 scores on POD 1 and POD 2 were significantly higher (P <0.001) in group L (165.5±3.8 vs 173.7±4.7) than those in group C (155.6±4.0 vs 163.2±4.5); and scores of physical comfort, emotional state, and pain in group L were superior to those in group C (P <0.05). In group L, patients possessed lower plasma concentration of pro-inflammatory factors (IL-6, TNF-α) and brain injury-related factors (S100B, NSE) (P <0.05), consumed less remifentanil and propofol, and experienced lower pain intensity. Multiple linear regression analysis demonstrated age and pain were correlated with postperative recovery quality.
Conclusion: Systemic lidocaine improved early recovery quality after supratentorial tumor resection with general anesthesia, and had certain brain-injury alleviation effects. These benefits may be attributed to the inflammation-alleviating and analgesic properties of lidocaine.
Keywords: brain neoplasm; brain protection; lidocaine; postoperative pain; recovery quality; supratentorial tumor resection.
© 2022 Zhao et al.
Conflict of interest statement
All authors have no conflicts of interest to report.
Figures
Similar articles
-
Effects of Systemic Lidocaine on Postoperative Recovery Quality and Immune Function in Patients Undergoing Laparoscopic Radical Gastrectomy.Drug Des Devel Ther. 2021 May 3;15:1861-1872. doi: 10.2147/DDDT.S299486. eCollection 2021. Drug Des Devel Ther. 2021. PMID: 33976537 Free PMC article.
-
Effect of Intravenous Lidocaine Infusion on Postoperative Early Recovery Quality in Upper Airway Surgery.Laryngoscope. 2021 Jan;131(1):E63-E69. doi: 10.1002/lary.28594. Epub 2020 Mar 2. Laryngoscope. 2021. PMID: 32119135 Clinical Trial.
-
Lidocaine Reduces Acute Postoperative Pain After Supratentorial Tumor Surgery in the PACU: A Secondary Finding From a Randomized, Controlled Trial.J Neurosurg Anesthesiol. 2016 Oct;28(4):309-15. doi: 10.1097/ANA.0000000000000230. J Neurosurg Anesthesiol. 2016. PMID: 26397235 Clinical Trial.
-
Association between perioperative intravenous lidocaine and subjective quality of recovery: A meta-analysis of randomized controlled trials.J Clin Anesth. 2021 Dec;75:110521. doi: 10.1016/j.jclinane.2021.110521. Epub 2021 Sep 20. J Clin Anesth. 2021. PMID: 34547603 Review.
-
Recent trends in the anesthetic management of craniotomy for supratentorial tumor resection.Curr Opin Anaesthesiol. 2016 Oct;29(5):552-7. doi: 10.1097/ACO.0000000000000365. Curr Opin Anaesthesiol. 2016. PMID: 27285727 Review.
Cited by
-
Efficacy of intraoperative systemic lidocaine on quality of recovery after laparoscopic colorectal surgery: a randomized controlled trial.Ann Med. 2024 Dec;56(1):2315229. doi: 10.1080/07853890.2024.2315229. Epub 2024 Feb 12. Ann Med. 2024. PMID: 38346397 Free PMC article. Clinical Trial.
-
Lidocaine attenuates TMZ resistance and inhibits cell migration by modulating the MET pathway in glioblastoma cells.Oncol Rep. 2024 May;51(5):72. doi: 10.3892/or.2024.8731. Epub 2024 Apr 12. Oncol Rep. 2024. PMID: 38606513 Free PMC article.
-
Tumor Necrosis Factor Alpha: Implications of Anesthesia on Cancers.Cancers (Basel). 2023 Jan 25;15(3):739. doi: 10.3390/cancers15030739. Cancers (Basel). 2023. PMID: 36765695 Free PMC article. Review.
-
Systemic Anti-Inflammatory Effects of Intravenous Lidocaine in Surgical Patients: A Systematic Review and Meta-Analysis.J Clin Med. 2023 May 31;12(11):3772. doi: 10.3390/jcm12113772. J Clin Med. 2023. PMID: 37297968 Free PMC article. Review.
-
Effects of perioperative intravenous lidocaine and esketamine on the quality of recovery and emotional state of patients after thyroidectomy: A randomised, double-blind, controlled trial.Indian J Anaesth. 2024 Apr;68(4):340-347. doi: 10.4103/ija.ija_1010_23. Epub 2024 Mar 13. Indian J Anaesth. 2024. PMID: 38586266 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous