Dual HDAC/BRD4 Inhibitors Relieves Neuropathic Pain by Attenuating Inflammatory Response in Microglia After Spared Nerve Injury
- PMID: 35501470
- PMCID: PMC9606187
- DOI: 10.1007/s13311-022-01243-6
Dual HDAC/BRD4 Inhibitors Relieves Neuropathic Pain by Attenuating Inflammatory Response in Microglia After Spared Nerve Injury
Abstract
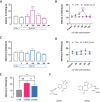
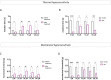
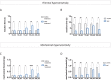
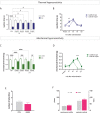
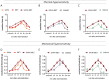
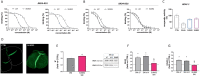
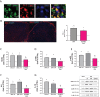
Despite the effort on developing new treatments, therapy for neuropathic pain is still a clinical challenge and combination therapy regimes of two or more drugs are often needed to improve efficacy. Accumulating evidence shows an altered expression and activity of histone acetylation enzymes in chronic pain conditions and restoration of these aberrant epigenetic modifications promotes pain-relieving activity. Recent studies showed a synergistic activity in neuropathic pain models by combination of histone deacetylases (HDACs) and bromodomain and extra-terminal domain (BET) inhibitors. On these premises, the present study investigated the pharmacological profile of new dual HDAC/BRD4 inhibitors, named SUM52 and SUM35, in the spared nerve injury (SNI) model in mice as innovative strategy to simultaneously inhibit HDACs and BETs. Intranasal administration of SUM52 and SUM35 attenuated thermal and mechanical hypersensitivity in the absence of locomotor side effects. Both dual inhibitors showed a preferential interaction with BRD4-BD2 domain, and SUM52 resulted the most active compound. SUM52 reduced microglia-mediated spinal neuroinflammation in spinal cord sections of SNI mice as showed by reduction of IBA1 immunostaining, inducible nitric oxide synthase (iNOS) expression, p65 nuclear factor-κB (NF-κB) and p38 MAPK over-phosphorylation. A robust decrease of the spinal proinflammatory cytokines content (IL-6, IL-1ß) was also observed after SUM52 treatment. Present results, showing the pain-relieving activity of HDAC/BRD4 dual inhibitors, indicate that the simultaneous modulation of BET and HDAC activity by a single molecule acting as multi-target agent might represent a promise for neuropathic pain relief.
Keywords: BET; Cytokines; HDAC; Microglia; NF-kB; Neuropathic pain.
© 2022. The Author(s).
Figures
Similar articles
-
Combined inhibition of histone deacetylases and BET family proteins as epigenetic therapy for nerve injury-induced neuropathic pain.Pharmacol Res. 2021 Mar;165:105431. doi: 10.1016/j.phrs.2021.105431. Epub 2021 Jan 30. Pharmacol Res. 2021. PMID: 33529752
-
Dual BET/HDAC inhibition to relieve neuropathic pain: Recent advances, perspectives, and future opportunities.Pharmacol Res. 2021 Nov;173:105901. doi: 10.1016/j.phrs.2021.105901. Epub 2021 Sep 20. Pharmacol Res. 2021. PMID: 34547384
-
N-terminal BET bromodomain inhibitors disrupt a BRD4-p65 interaction and reduce inducible nitric oxide synthase transcription in pancreatic β-cells.Front Endocrinol (Lausanne). 2022 Sep 13;13:923925. doi: 10.3389/fendo.2022.923925. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36176467 Free PMC article.
-
Histone deacetylase as emerging pharmacological therapeutic target for neuropathic pain: From epigenetic to selective drugs.CNS Neurosci Ther. 2024 May;30(5):e14745. doi: 10.1111/cns.14745. CNS Neurosci Ther. 2024. PMID: 38715326 Free PMC article. Review.
-
Histone deacetylase 3 (HDAC 3) as emerging drug target in NF-κB-mediated inflammation.Curr Opin Chem Biol. 2016 Aug;33:160-8. doi: 10.1016/j.cbpa.2016.06.019. Epub 2016 Jun 29. Curr Opin Chem Biol. 2016. PMID: 27371876 Free PMC article. Review.
Cited by
-
Potential Therapeutic Effects of Short-Chain Fatty Acids on Chronic Pain.Curr Neuropharmacol. 2024;22(2):191-203. doi: 10.2174/1570159X20666220927092016. Curr Neuropharmacol. 2024. PMID: 36173071 Free PMC article. Review.
-
Global research trends on epigenetics and neuropathic pain: A bibliometric analysis.Front Mol Neurosci. 2023 Apr 19;16:1145393. doi: 10.3389/fnmol.2023.1145393. eCollection 2023. Front Mol Neurosci. 2023. PMID: 37152435 Free PMC article. Review.
-
The Epigenetics of Neuropathic Pain: A Systematic Update.Int J Mol Sci. 2023 Dec 5;24(24):17143. doi: 10.3390/ijms242417143. Int J Mol Sci. 2023. PMID: 38138971 Free PMC article. Review.
-
Bromodomain-containing protein 4 contributes to chronic postsurgical pain via activating TLR4/NF-kappaB-dependent neuroinflammation.BMC Anesthesiol. 2025 Jul 12;25(1):346. doi: 10.1186/s12871-025-03216-6. BMC Anesthesiol. 2025. PMID: 40652178 Free PMC article.
-
Development of Potent Dual BET/HDAC Inhibitors via Pharmacophore Merging and Structure-Guided Optimization.ACS Chem Biol. 2024 Feb 16;19(2):266-279. doi: 10.1021/acschembio.3c00427. Epub 2024 Jan 31. ACS Chem Biol. 2024. PMID: 38291964 Free PMC article.
References
-
- Van Hecke O, Austin SK, Khan RA, Smith BH, Torrance N. Neuropathic pain in the general population: a systematic review of epidemiological studies. Pain. 2014;155:654–662. - PubMed
-
- Alles SRA, Smith PA. Etiology and pharmacology of neuropathic pain. Pharmacol Rev. 2018;70(2):315–347. - PubMed
-
- Finnerup NB, Kuner R, Jensen TS. Neuropathic pain: from mechanisms to treatment. Physiol Rev. 2021;101(1):259–301. - PubMed
-
- Mathieson S, Kasch R, Maher CG, Zambelli Pinto R, McLachlan AJ, Koes BW, et al. Combination Drug therapy for the management of low back pain and sciatica: systematic review and meta-analysis. J Pain. 2019;20:1–15. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

